Key Takeaways
- The narcissist brain shows measurable structural differences, including reduced cortical thickness in the insular cortex — the region responsible for empathy processing and emotional awareness.
- Narcissistic individuals retain cognitive empathy (understanding what others feel) while showing significant deficits in affective empathy (feeling what others feel) — a dissociation that explains why someone can describe your pain perfectly while doing nothing to stop causing it.
- Prefrontal cortex dysfunction in narcissistic personality disorder compromises self-regulation, impulse control, and the capacity for accurate social cognition — creating a brain that strategizes brilliantly but cannot modulate its own interpersonal behavior.
- Frontolimbic connectivity disruptions between the prefrontal cortex and amygdala produce the emotional volatility and rapid escalation that make every conversation feel like it could detonate without warning.
- Neuroplasticity research indicates that narcissistic brain patterns are not permanently fixed; targeted interventions can promote measurable reorganization of empathy-related neural circuits — though the individual must sustain engagement with the process.
If you are reading this at 2am, searching for some neurological explanation for the person who can read your emotions with surgical precision but seems incapable of actually caring about them — you are not imagining things. The narcissist brain is structurally and functionally distinct from the neurotypical brain in ways that modern neuroimaging has made impossible to dismiss. The confusion you feel — how can someone understand me so completely and hurt me so consistently — has a concrete answer in the architecture of the brain itself.

Narcissistic personality disorder is not simply a collection of difficult behaviors. It is rooted in measurable differences in cortical thickness, prefrontal regulation, and the neural circuits that produce empathy. Understanding these differences will not undo the damage. But it will explain why your attempts to reach the person kept failing — and why that failure was never about your effort.
In over two decades of clinical work, I have seen the same pattern hundreds of times: someone walks in exhausted, carrying years of trying to love a person whose brain is structurally unable to receive that love in the way it was intended. They want to know if the person can change, if something is genuinely wrong, or if they themselves are the problem. The neuroscience answers all three questions — and the answers are more nuanced, and more useful, than the labels suggest.
What Does the Narcissist Brain Look Like on Neuroimaging?
Brain imaging studies have revealed that individuals diagnosed with narcissistic personality disorder exhibit reduced gray matter volume and cortical thickness in regions directly responsible for empathy, emotional regulation, and self-awareness. The most consistent finding across multiple neuroimaging studies is structural compromise in the insular cortex — a deep cortical region that integrates bodily sensations with emotional awareness and enables a person to recognize and resonate with another individual’s internal state.

A landmark study published in the Journal of Psychiatric Research (Schulze et al., 2013) used voxel-based morphometry to demonstrate that individuals with narcissistic personality disorder had significantly less gray matter in the left anterior insula compared to healthy controls. The anterior insula is the region most strongly associated with compassion, disgust recognition, and the felt sense of another person’s suffering. When this area is structurally thinner, the brain’s capacity to generate empathic resonance is physically diminished.
What this means in practical terms — in the terms that matter when you are living with someone whose empathy feels performative — is that the signal genuinely does not arrive with the same fidelity. The right anterior insula, which contributes to interoceptive awareness, also shows reduced activation in narcissistic individuals. This creates a double deficit: the narcissist brain struggles both to read its own emotional landscape accurately and to model the emotional experience of others. What appears externally as indifference is often, at the neural level, a perceptual gap. The person is not choosing to ignore your pain. Their brain is failing to register it at the intensity you are transmitting it.
In my practice, I frequently explain this distinction to clients who have spent years personalizing the empathy gap — believing they were not important enough, not articulate enough, not worth the effort. The insula finding reframes the entire dynamic. The deficit is structural. It was never about your value.
How Does Prefrontal Cortex Dysfunction Drive Narcissistic Behavior?
The prefrontal cortex governs executive function, impulse control, long-range planning, and the capacity to evaluate one’s own behavior from another person’s perspective — a process neuroscientists call mentalizing or theory of mind. In narcissistic personality disorder, both the medial prefrontal cortex and the dorsolateral prefrontal cortex show functional abnormalities that directly account for the behavioral hallmarks of the condition.
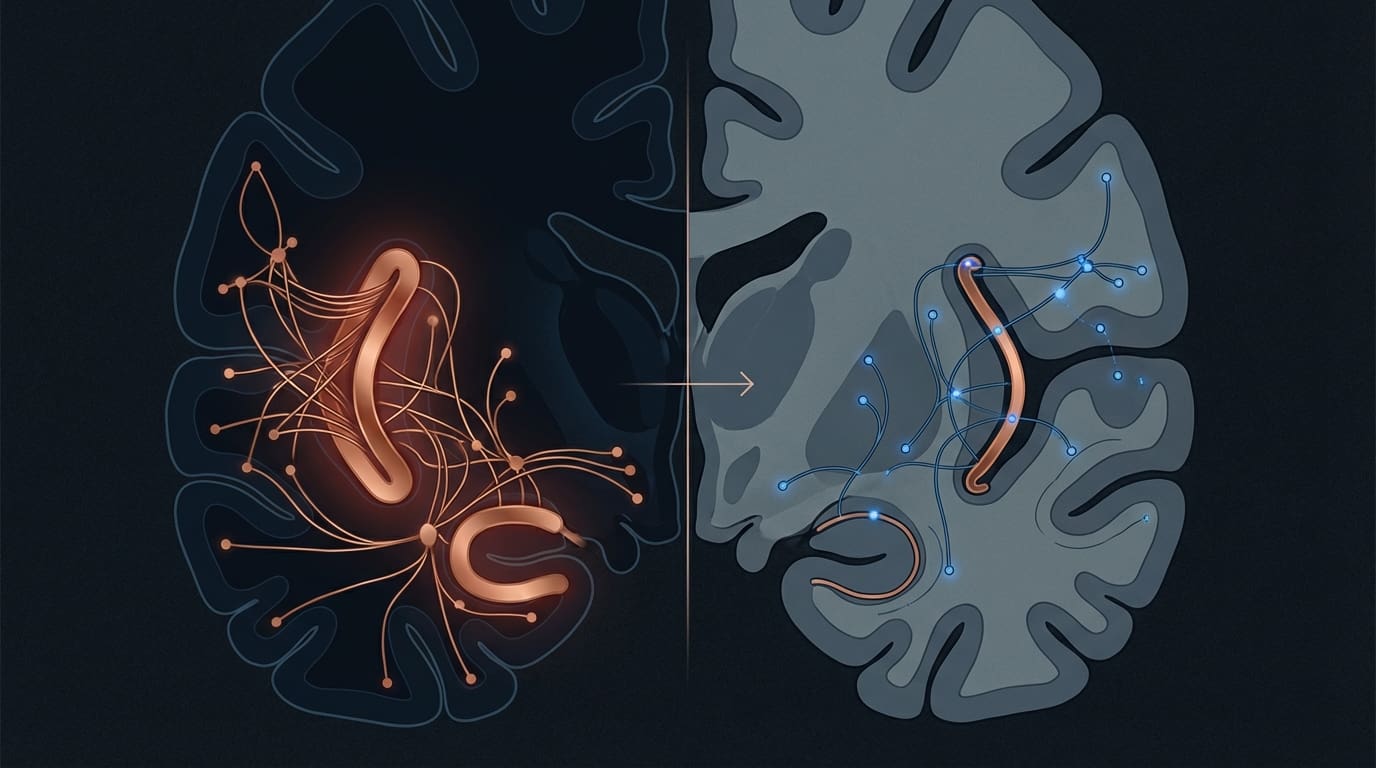
The medial prefrontal cortex is the brain’s primary seat of self-referential processing. Research published in Neuroscience & Biobehavioral Reviews has demonstrated that narcissistic individuals show hyperactivation in medial PFC regions during self-focused tasks but markedly reduced activation when asked to consider another person’s perspective (Cascio et al., 2015). This asymmetry is not a choice — it is a default network configuration. The narcissist brain is, in a measurable sense, wired to prioritize self-relevant information at the expense of other-relevant information.
The dorsolateral prefrontal cortex, responsible for cognitive flexibility and behavioral regulation, shows complementary dysfunction. When this region underperforms, the individual struggles to inhibit impulsive self-serving behavior, to adapt their approach based on social feedback, and to hold multiple perspectives simultaneously. I frequently observe this in high-functioning individuals who are extraordinarily capable in strategic domains but consistently fail to modulate interpersonal behavior — the dorsolateral PFC can execute complex planning while the medial PFC remains locked in self-referential mode. These are often the people whose partners describe the same bewildering experience: brilliant at work, devastating at home.
The Frontolimbic Disconnect
Perhaps the most consequential structural finding involves the connectivity between the prefrontal cortex and the amygdala — the brain’s threat-detection and emotional-intensity center. In narcissistic personality disorder, functional connectivity between these regions is disrupted. The amygdala generates emotional responses — rage, envy, perceived threat to status — that the prefrontal cortex cannot adequately regulate.
If you have ever watched someone articulate exactly what the right response should be and then do the opposite under pressure, you have witnessed frontolimbic disconnect in real time. The knowledge exists. The regulatory pathway to translate that knowledge into behavior under emotional load does not function reliably. This is one of the most painful aspects for people living with narcissistic individuals — the proof that they know better makes the failure to do better feel intentional. At the neural level, it is not intentional. It is architectural.
Why Can Narcissists Understand Emotions Without Feeling Them?
This is the question that brings most people to an article like this. The person in your life can tell you exactly what you are feeling — sometimes before you have fully articulated it yourself. They can describe your emotional state with remarkable accuracy. And then they can act as if that information carries no weight whatsoever. The cruelty of it is that it looks like a choice. The neuroscience reveals it as a structural dissociation.
The empathy deficit in narcissistic personality disorder is not a total absence — it is a specific split between two neurologically distinct empathy systems. Cognitive empathy, the ability to intellectually model what another person is thinking or feeling, remains largely intact and is sometimes even enhanced. Affective empathy, the visceral, felt-sense experience of resonating with another person’s emotional state, is significantly diminished.
Cognitive empathy relies heavily on the temporoparietal junction and dorsomedial prefrontal cortex — regions involved in perspective-taking and mental modeling. These areas function normally or even show heightened activation in narcissistic individuals, which is why many people with narcissistic traits are skilled at reading others with precision. Affective empathy, by contrast, depends on the mirror neuron system, the anterior insula, and the anterior cingulate cortex. A study by Ritter et al. (2011) demonstrated that narcissistic individuals showed significantly reduced activation in these regions when exposed to others’ emotional distress.
In my clinical work, I see two kinds of people searching for information about the narcissist brain — those trying to understand someone who hurt them, and those quietly terrified that it might describe themselves. Both deserve clarity, not labels. For the first group, the cognitive-affective split explains the maddening paradox: the knowledge is there, the resonance is not. For the second group, the fact that you are concerned about your own empathy capacity is itself a meaningful neurological signal — one that suggests your affective circuits are more engaged than you fear.
Can the Narcissist Brain Be Rewired Through Neuroplasticity?
The brain’s capacity for structural and functional reorganization — neuroplasticity — does not exempt narcissistic neural patterns. While the research on neuroplasticity-based interventions for narcissistic personality disorder specifically is still in early stages, converging evidence from adjacent fields provides substantial grounds for measured optimism.
Longitudinal studies on empathy training have demonstrated that targeted practice in perspective-taking and compassion-focused exercises can increase gray matter density in the anterior insula and anterior cingulate cortex — the same regions that show structural deficits in narcissistic personality disorder. Research conducted at the Max Planck Institute (Klimecki et al., 2013) documented measurable increases in insula activation and gray matter volume following structured compassion training programs lasting as little as three months.
Prefrontal regulation capacity is equally plastic. Cognitive behavioral interventions, mindfulness-based approaches, and real-time neurofeedback protocols have all demonstrated the capacity to strengthen prefrontal-amygdala connectivity — the frontolimbic pathway most disrupted in narcissistic personality disorder. The key variable is not whether the brain can change but whether the individual can sustain engagement with the process long enough for reorganization to consolidate.
This is where my approach differs from most clinical frameworks. Traditional interventions attempt to change narcissistic behavior through retrospective conversation — discussing events days or weeks after they occurred, when the emotional circuitry that drove the behavior is no longer active. Real-Time Neuroplasticity operates on a fundamentally different principle: engaging the brain’s plasticity mechanisms during moments of genuine emotional activation, when the circuits in question are online and accessible to restructuring. The difference in outcomes is substantial, and it is the reason I work the way I do — embedded in real-time rather than confined to a weekly hour.
Whether you are trying to understand someone else’s narcissistic patterns or examining your own, the neuroplasticity evidence means the same thing: the architecture is not destiny. But changing it requires precision about which circuits need restructuring and sustained access to the conditions under which restructuring actually occurs. A strategy call is where that precision begins — mapping the specific neural profile and determining whether a targeted approach can produce the structural change that other methods have not.
What Role Does the Reward System Play in Narcissistic Patterns?
The mesolimbic dopamine pathway — the brain’s core reward circuit — shows distinct activation patterns in narcissistic personality disorder that help explain why narcissistic behavior is so resistant to change through willpower alone. Narcissistic supply — admiration, status confirmation, interpersonal dominance — activates the ventral striatum and nucleus accumbens in patterns closely analogous to substance reward.
This means that narcissistic behavior is not merely habitual — it is neurochemically reinforced. Each instance of received admiration or successful manipulation produces a dopamine response that strengthens the very circuits driving the behavior. The narcissist brain is, in this respect, caught in a self-reinforcing loop: the behavior generates the neurochemical reward that makes the behavior more likely to recur.
If you have been on the receiving end of this loop, you already know what it looks like from the outside — the constant need for validation, the inability to sustain satisfaction, the escalation when supply is withdrawn. What you may not have understood is that the person is not choosing this pattern any more than someone with a substance dependency is choosing their next use. The dopaminergic reinforcement is real, measurable, and powerful.
Breaking this loop requires not just insight but actual reward-system recalibration. The brain must develop alternative sources of dopaminergic activation — connection, contribution, authentic relational engagement — that can gradually compete with and eventually replace the narcissistic supply pathway. This is achievable, but it requires sustained, structured intervention that engages the brain’s plasticity mechanisms during moments of genuine emotional activation — not in retrospective conversation about those moments days or weeks later. In my experience, reward-system recalibration is the longest phase of the work, and it is the phase where most conventional approaches fail because they cannot maintain real-time engagement with the circuit long enough for the alternative pathways to consolidate.
References
1. Schulze, L., Dziobek, I., Vater, A., Heekeren, H. R., Bajbouj, M., Renneberg, B., Heuser, I., & Roepke, S. (2013). Gray matter abnormalities in patients with narcissistic personality disorder. Journal of Psychiatric Research, 47(10), 1363–1369. https://pubmed.ncbi.nlm.nih.gov/23465295/
2. Cascio, C. N., Konrath, S. H., & Falk, E. B. (2015). Narcissists’ social pain seen only in the brain. Neuroscience & Biobehavioral Reviews, 55, 567–579. https://doi.org/10.1016/j.neubiorev.2014.11.018
3. Ritter, K., Dziobek, I., Preissler, S., Rüter, A., Vater, A., Fydrich, T., Lammers, C. H., Heekeren, H. R., & Roepke, S. (2011). Lack of empathy in patients with narcissistic personality disorder. Psychiatry Research, 187(1-2), 241–247. https://pubmed.ncbi.nlm.nih.gov/20570110/
4. Klimecki, O. M., Leiberg, S., Ricard, M., & Singer, T. (2013). Differential pattern of functional brain plasticity after compassion and empathy training. Social Cognitive and Affective Neuroscience, 9(6), 873–879. https://doi.org/10.1093/cercor/bhs142
What the First Conversation Looks Like
You have probably already tried to understand the person who hurt you. You may have read every article, watched every video, and diagnosed the pattern from a distance. And yet the understanding did not produce relief — because knowing what narcissistic personality disorder looks like does not explain why your specific experience felt the way it did, or what to do with the wreckage it left behind.
The first conversation with Dr. Ceruto starts somewhere different. Rather than cataloging symptoms or revisiting relational history, she maps the neural architecture driving the pattern you are dealing with — whether that pattern belongs to someone in your life or to circuitry you recognize in yourself. The conversation identifies which circuits are underperforming, which are compensating, and where the brain’s plasticity mechanisms offer the most leverage for genuine reorganization. It is direct, grounded in the same neuroscience you just read, and designed to answer the question that brought you here: can this actually change, and what would it take?
This is a strategy call — one hour with Dr. Ceruto, focused entirely on understanding the neurological root of the pattern and whether MindLAB’s Real-Time Neuroplasticity methodology can produce the structural change that other approaches have not.
Frequently Asked Questions
Is the narcissist brain permanently different from a typical brain?
The narcissist brain shows measurable structural differences — including reduced insular cortex thickness and prefrontal dysfunction — but these differences are not permanent in the way that a fixed anatomical defect would be. Neuroplasticity research demonstrates that gray matter density in empathy-related regions can increase with sustained, targeted intervention. The brain’s architecture reflects its history of use, and that history can be rewritten through structured engagement that activates the specific circuits requiring reorganization.
Can brain scans diagnose narcissistic personality disorder?
Brain imaging cannot currently serve as a standalone diagnostic tool for narcissistic personality disorder because the structural differences observed in research studies represent group-level statistical patterns rather than individual-level diagnostic thresholds. However, neuroimaging findings — particularly reduced anterior insula volume and disrupted frontolimbic connectivity — provide critical biological context that strengthens diagnostic confidence when combined with behavioral assessment and detailed clinical history.
Why do narcissists seem to understand emotions but not care about them?
Narcissistic individuals retain cognitive empathy — the ability to intellectually model another person’s emotional state — while showing significant deficits in affective empathy, which depends on mirror neuron and anterior insula activation to produce felt emotional resonance. The cognitive system, anchored in the temporoparietal junction, allows accurate reading of others’ emotions. The affective system, dependent on the insula and anterior cingulate cortex, fails to translate that understanding into shared feeling. This is why the person can describe your pain accurately and still not be moved by it.
What is the relationship between narcissism and the brain’s reward system?
Narcissistic supply — admiration, status confirmation, interpersonal control — activates the mesolimbic dopamine pathway in patterns that closely mirror substance reward, producing ventral striatum and nucleus accumbens responses that neurochemically reinforce the behavior. This reward-system involvement explains why narcissistic patterns resist change through insight alone: the behavior is not merely habitual but is actively maintained by dopaminergic reinforcement that makes each successful instance more likely to recur.
Can someone with narcissistic brain patterns recognize the problem in themselves?
Self-recognition is neurologically possible but structurally disadvantaged. The medial prefrontal cortex hyperactivation that characterizes narcissistic personality disorder biases the brain toward self-enhancing interpretations, making accurate self-assessment genuinely harder at the circuit level. However, individuals who do recognize the pattern — often prompted by relational consequences severe enough to override the self-enhancement bias — represent the strongest candidates for neuroplasticity-based intervention, because their recognition signals that the evaluative circuits are at least partially online.






