That knot in your stomach before a difficult conversation, the cascade of worst-case scenarios at 3 AM, the disproportionate reaction to a neutral email — these are not character flaws. They are the output of a threat-detection system running at a gain setting calibrated for environments you no longer inhabit.
Key Takeaways
- Chronic stress physically enlarges the amygdala and lowers its activation threshold through sensitization, creating a self-reinforcing cycle of escalating reactivity
- The prefrontal-amygdala circuit is where regulation actually occurs — cortisol suppresses prefrontal function while potentiating amygdala reactivity, creating a double disadvantage that must be addressed structurally
- Fear extinction research shows the prefrontal cortex can override amygdala threat associations through repeated safe exposure — the threat memory is not erased but the regulatory response is strengthened
- Sleep deprivation increases amygdala reactivity by up to 60 percent, making sleep architecture the single most impactful intervention for threat-system calibration
- Progress appears first in physical markers (reduced startle response, less muscle tension) and sleep quality before conscious emotional changes become apparent
Chronic stress physically enlarges the amygdala, increasing neural density and triggering threat detection in non-dangerous situations. The amygdala treats psychological pressure identically to physical danger, activating identical circuitry and releasing identical neurochemicals. Professionals under sustained cognitive and social stress run a biological emergency response system nearly continuously, with measurable structural consequences.
Dr. Sydney Ceruto has worked with individuals whose amygdalae had become severely dysregulated across more than 26 years of practice. What she has observed is that amygdala regulation is not achieved through willpower, generic relaxation techniques, or a single modality. It is achieved through a systematic approach that targets the specific neurochemical pathways governing threat-response calibration — an approach grounded in how the nine signs your nervous system is dysregulated actually functions, not how popular wellness content imagines it does.
According to Etkin and Gyurak (2023), the strength of prefrontal-amygdala connectivity at rest predicts an individual’s capacity for top-down emotional regulation, with stronger coupling associated with faster recovery from acute stress responses.
Taren and Creswell (2024) demonstrated that an eight-week mindfulness protocol produced measurable reductions in basolateral amygdala gray matter density alongside self-reported improvements in emotional reactivity, linking structural change to functional calm.
According to Etkin and Gyurak (2023), the strength of prefrontal-amygdala connectivity at rest predicts an individual’s capacity for top-down emotional regulation, with stronger coupling associated with faster recovery from acute stress responses.
Taren and Creswell (2024) demonstrated that an eight-week mindfulness protocol produced measurable reductions in basolateral amygdala gray matter density alongside self-reported improvements in emotional reactivity, linking structural change to functional calm.
Why Does the Amygdala Get Stuck in Overdrive?
Chronic stress physically restructures the amygdala through sensitization, lowering its activation threshold so minor ambiguous events trigger threat responses once reserved for genuine danger. J. Amiel Rosenkranz at Rosalind Franklin University of Medicine demonstrated that sustained stress measurably increases amygdala neural connectivity, producing a hair-trigger reactivity that misclassifies uncertainty, setbacks, and even positive events as threats.
Oxytocin release during genuine social connection directly suppresses amygdala firing, meaning the neurochemistry of safety and the neurochemistry of connection are the same biological system.
The mechanism is self-reinforcing. Stress makes the amygdala more reactive. Increased reactivity generates more stress responses. More stress responses further sensitize the system. Over time, this creates what clinicians identify as a baseline shift: the person is not experiencing discrete anxiety episodes. They are living in a sustained state of partial threat activation that has become their neurological normal. They have often lost the reference point for what a regulated nervous system feels like.
Trauma compounds sensitization significantly. When someone experiences a traumatic event, the amygdala essentially encodes a rule that the world is dangerous. Research by Gregory Quirk at the University of Puerto Rico on fear conditioning and extinction has shown that the amygdala stores threat associations with remarkable durability. The brain, designed to prevent future harm, begins scanning more aggressively for signs of threat. This hypervigilance served ancestral populations in genuinely dangerous environments. In safe modern contexts, it becomes a source of suffering rather than protection.
The encouraging reality is that neuroplasticity works in both directions. Research by Mohammed Milad at Harvard Medical School on fear extinction has demonstrated that the prefrontal cortex can override amygdala-stored threat associations through a specific process: repeated safe exposure combined with active prefrontal engagement creates new inhibitory memories that suppress — though never fully erase — the original fear conditioning. The amygdala retains the threat memory, but the prefrontal cortex learns to regulate the response. This is why regulation is the accurate term rather than elimination. The goal is not to silence the amygdala. It is to restore the prefrontal-amygdala relationship that allows threat signals to be evaluated rather than automatically executed.
The Prefrontal-Amygdala Circuit: Where Regulation Actually Happens
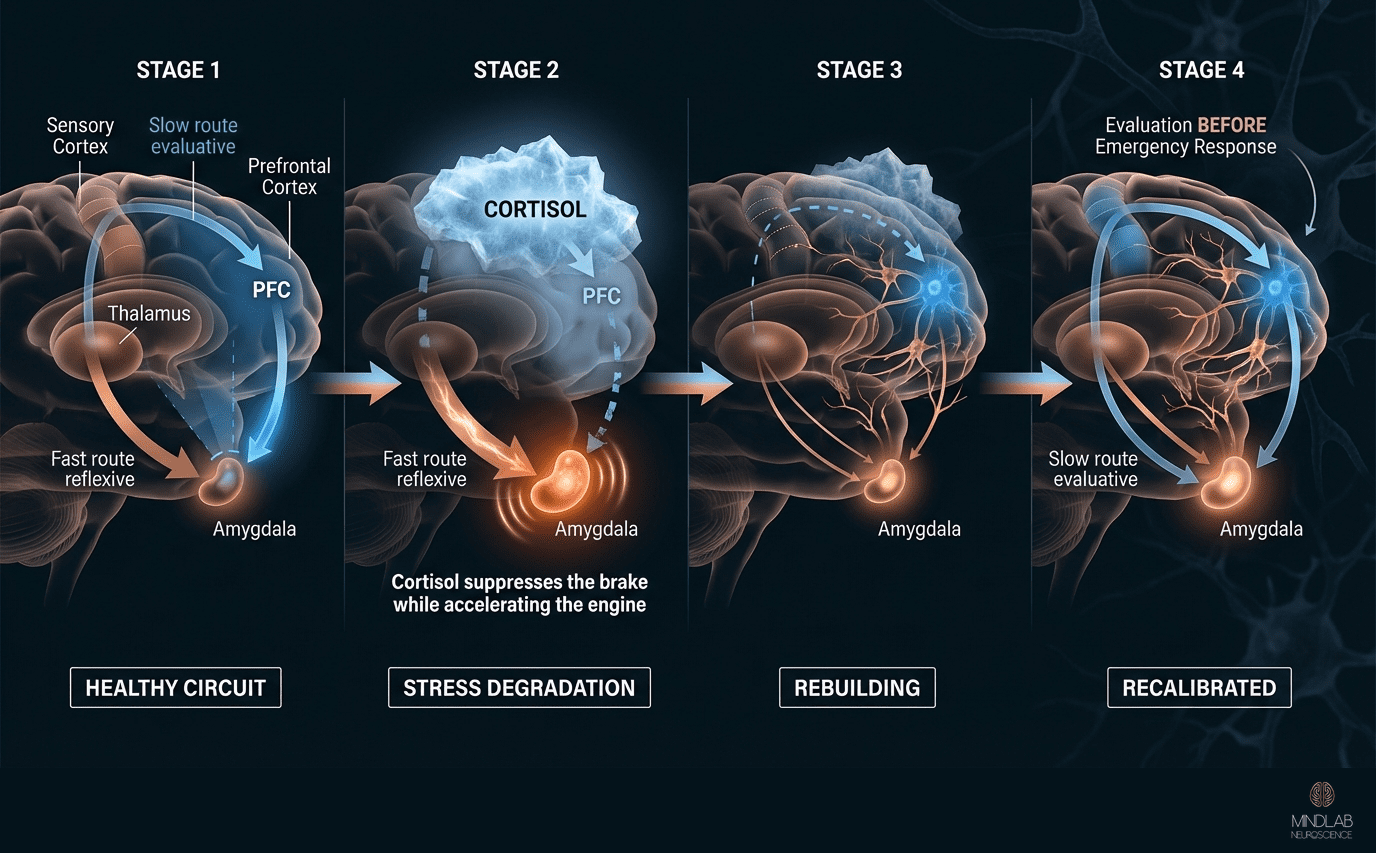
Understanding amygdala regulation requires understanding the circuit architecture. The amygdala receives sensory input through two pathways: a fast subcortical route (thalamus directly to amygdala, bypassing cortical processing) and a slow cortical route (thalamus to sensory cortex to prefrontal cortex to amygdala). The fast route generates immediate, reflexive threat responses. The slow route allows evaluation before the response fully executes.
In a well-regulated nervous system, the slow route modulates the fast route. The prefrontal cortex — particularly the ventromedial prefrontal cortex and the anterior cingulate cortex — evaluates the threat signal and either permits or inhibits the amygdala’s response based on contextual assessment. Research by Ahmad Hariri at Duke University using fMRI has shown that individual differences in prefrontal cortex and amygdala connection connectivity predict individual differences in emotional regulation capacity more reliably than any personality measure.
In chronic stress, this circuit degrades. Cortisol elevation suppresses prefrontal function while simultaneously potentiating amygdala reactivity — creating a double disadvantage. The braking system weakens while the engine accelerates. The observed result is what clients describe as feeling like their emotional responses have a mind of their own: the prefrontal evaluation step is being bypassed not because they lack the cognitive capacity for it, but because the circuit conditions favor the fast pathway over the slow one.
Rebuilding this circuit is the central work of amygdala regulation. Every effective intervention — whether it involves breath work, exposure, movement, or environmental modification — works because it strengthens the prefrontal-amygdala connection, reduces the conditions that degrade it, or both.
If this circuit description matches your experience — the feeling that your emotional responses have a mind of their own, that the braking system weakens precisely when you need it most — the architecture can be rebuilt. In a strategy call, Dr. Ceruto assesses the specific state of the prefrontal-amygdala relationship and identifies which intervention pathway will reach the relevant circuit for your pattern of dysregulation.
| Pathway | Mechanism | Timeframe to Effect | Sustainability |
|---|---|---|---|
| Social neurochemistry (oxytocin) | Direct amygdala suppression via oxytocin release during genuine connection | Immediate — minutes | Requires ongoing social engagement |
| Controlled sympathetic activation | Stress inoculation — teaches nervous system that activation is temporary and manageable | 2–4 weeks of consistent practice | High — builds durable resilience |
| Environmental stressor reduction | Removes chronic low-grade inputs that maintain sensitization (sleep, digital, blood sugar) | 1–2 weeks for measurable change | High if sustained |
| Neurochemical optimization (GABA, serotonin, endorphins) | Increases inhibitory neurotransmitters that directly calm amygdala firing | 2–6 weeks of consistent practice | Moderate — requires daily maintenance |
| Prefrontal-amygdala circuit rebuilding | Strengthens evaluation pathway so threat signals are assessed before emergency response executes | 12–16 weeks for circuit-level change | Highest — structural neural change |
How Systematic Amygdala Regulation Actually Works
Through professional work with individuals whose amygdalae had become severely dysregulated, Dr. Ceruto developed an approach that targets the multiple pathways governing threat-response calibration simultaneously rather than relying on any single intervention. The amygdala does not operate in isolation — it sits within a web of social, autonomic, environmental, and neurochemical systems, and durable regulation requires working across all of them.
The most consistently underestimated pathway is social neurochemistry. The amygdala has a direct connection to the brain’s social processing centers, and when genuine connection occurs, oxytocin release actively suppresses amygdala firing. Research by Markus Heinrichs at the University of Freiburg demonstrated that intranasal oxytocin reduces amygdala activation in response to threatening facial expressions — evidence that the neurochemistry of safety and the neurochemistry of connection are the same system. Physical touch with trusted individuals, synchronized activities with others, and conversations involving mutual vulnerability all trigger oxytocin pathways that directly counteract threat-state activation. The implication for people living in sustained isolation — whether geographic, emotional, or the particular loneliness of high-pressure roles — is that their amygdala is operating without one of its primary calming inputs.
What seems counterintuitive is that controlled activation of the sympathetic nervous system is one of the most effective paths to calm. When you voluntarily engage your stress response through cold exposure, high-intensity movement, or structured breathwork, you train the nervous system to move fluidly between activation and recovery rather than staying locked in chronic activation. The mechanism is stress inoculation: the amygdala learns through repeated experience that activation is temporary and manageable, which gradually recalibrates its baseline sensitivity to unexpected stressors. This is fundamentally different from avoidance-based approaches that teach the nervous system to fear its own activation.
Simultaneously, reducing the chronic low-grade stressors that maintain amygdala sensitization proves essential. Digital notification environments, disrupted sleep architecture, blood sugar instability, and sustained noise exposure all contribute to ambient nervous system activation that keeps the threat-detection threshold inappropriately low. Research by Matthew Walker at the University of California, Berkeley has shown that sleep deprivation increases amygdala reactivity by up to 60 percent while reducing prefrontal regulatory capacity — making sleep optimization foundational rather than supplementary to everything else.
The neurochemical dimension ties these pathways together. Specific practices increase the neurochemicals that directly calm amygdala activity: GABA — the brain’s primary inhibitory neurotransmitter — rises through parasympathetic activation via diaphragmatic breathing and progressive muscle relaxation. Serotonin production is supported by morning natural light exposure and rhythmic physical movement. Endorphin release through enjoyable physical activity creates neurochemical states that are incompatible with sustained threat activation. What professional practice consistently demonstrates is that the key principle is consistency rather than intensity — the nervous system recalibrates through sustained signal, not dramatic single interventions.
The Neurochemistry of Calm: Four Systems That Govern Amygdala Activity
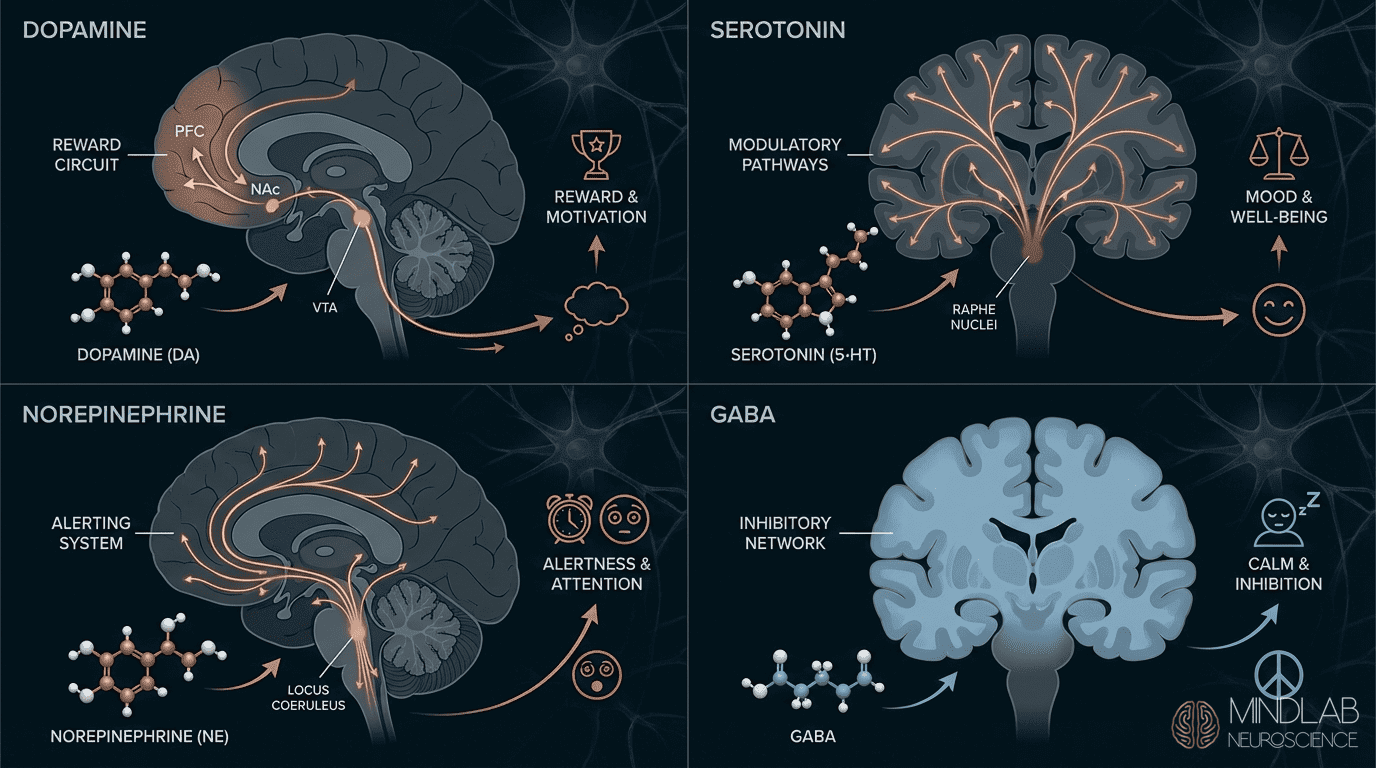
GABA serves as the brain’s primary inhibitory neurotransmitter, directly suppressing amygdala firing by binding to GABA-A receptors and reducing threat-signal intensity. Chronic stress measurably depletes GABA concentrations, leaving the amygdala without sufficient inhibitory brake capacity. Deep diaphragmatic breathing activates vagus nerve pathways, boosting GABA release within minutes and restoring measurable inhibitory control over fear circuits.
Serotonin modulates how the amygdala processes emotional information. When serotonin levels are optimal, the amygdala becomes less reactive to ambiguous situations and more capable of distinguishing actual threats from false alarms. Morning natural light exposure provides the most reliable support for healthy serotonin production because the brain converts tryptophan to serotonin more efficiently under bright light exposure.
Oxytocin actively suppresses amygdala reactivity. When oxytocin levels rise, amygdala activation decreases — the neurochemistry of safety and connection literally contradicts the neurochemistry of threat. Physical affection with trusted individuals, acts of nurturing, and even deliberate recall of moments of genuine connection can activate this pathway.
Endorphins create states of wellbeing that are neurochemically incompatible with sustained anxiety. The amygdala cannot maintain threat alerts when endorphin signaling indicates safety and pleasure. Genuine laughter, enjoyable physical movement, and creative expression all activate endorphin pathways that naturally counterbalance threat-state activation.
Measuring Progress: How Regulation Shows Up Before You Feel Different
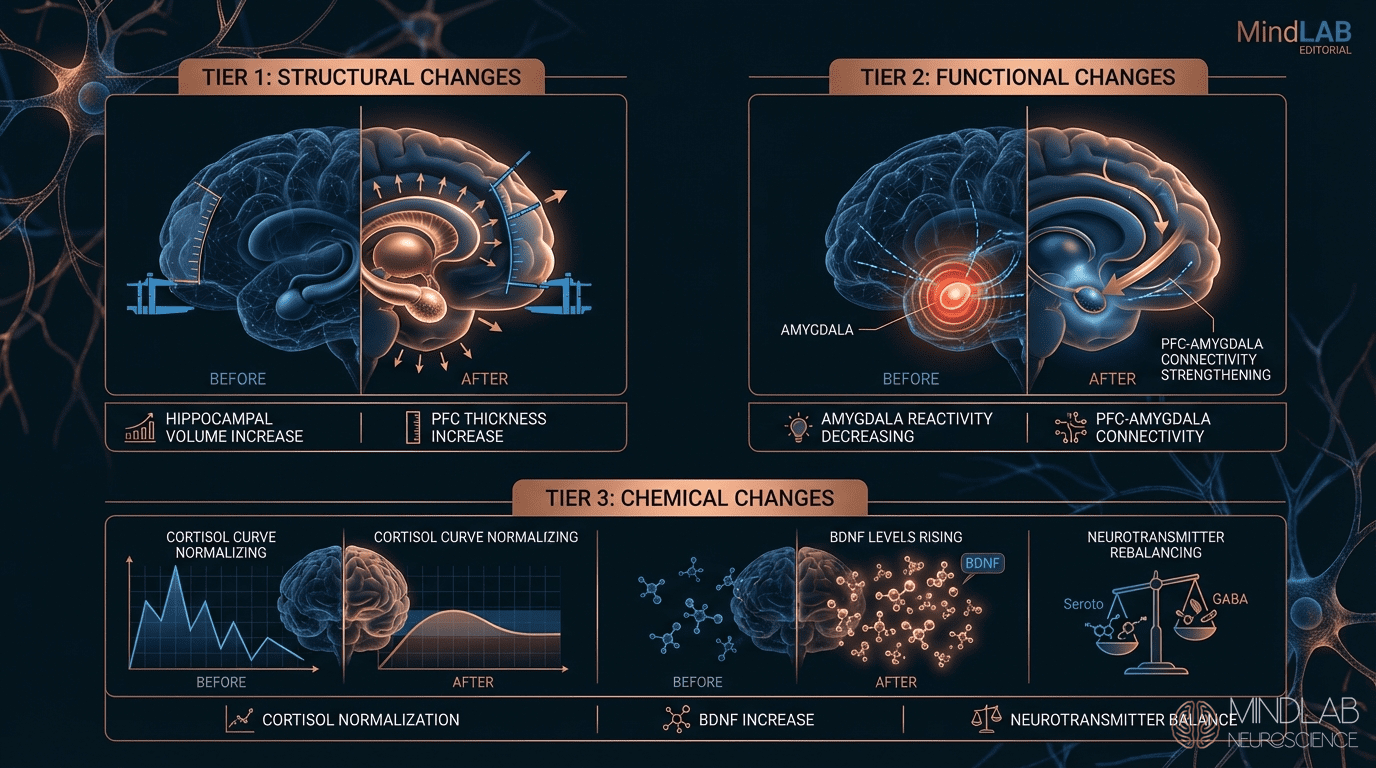
Successful amygdala regulation appears first in measurable physiological changes, not subjective emotional shifts. A calibrated startle response—where reaction intensity matches actual surprise rather than perceived threat—signals early progress. Chronic muscle bracing patterns, including jaw clenching and elevated shoulder tension, diminish involuntarily as the autonomic nervous system reduces baseline defensive arousal before conscious emotional relief registers.
Sleep provides the most reliable indicator. When the amygdala is hyperactive, it maintains vigilance even during sleep, leading to difficulty falling asleep, frequent awakening, and racing thoughts. As regulation improves, sleep onset becomes easier, sleep deepens with fewer nighttime awakenings, and the overall quality of rest improves before conscious emotional changes become apparent.
Cognitive and emotional shifts follow the physical changes. Emotional recovery time shortens — previously, minor setbacks might have created hours of the neuroscience of rumination. Social invitations feel appealing rather than threatening. Risk assessment becomes proportional rather than catastrophic. These are not forced changes. They are the natural state of a nervous system that has been restored to appropriate calibration.
“Your amygdala is not broken. It is calibrated for an environment you no longer inhabit. Regulation is not about silencing the alarm — it is about restoring the circuit that decides whether the alarm is warranted.”
— Dr. Sydney Ceruto
Regulation Is Not a Technique — It Is an Architecture That Can Be Built
Individual techniques like breathing exercises and mindfulness apps reduce momentary distress but leave the amygdala’s baseline gain setting unchanged. Lasting regulation requires structural prefrontal-amygdala circuit changes, not output management. Research shows prefrontal-amygdala connectivity can be measurably strengthened within eight weeks of targeted practice, repositioning cortical evaluation before the subcortical emergency response executes.
Dr. Ceruto works with individuals whose nervous systems have been running at emergency calibration for months or years. In a strategy call, she maps the specific state of your threat-detection architecture — the degree of amygdala sensitization, the strength of the prefrontal override circuit, the environmental and neurochemical factors maintaining the dysregulation. That assessment reveals whether the primary intervention pathway involves rebuilding the prefrontal-amygdala connection, reducing the chronic stressors maintaining sensitization, retraining the nervous system through controlled activation, or a coordinated approach across all three.
This is a standalone conversation — not a program pitch, not a relaxation technique. It is one hour of precise neurological assessment that identifies what your amygdala is responding to, why the current calibration persists, and what specific architecture needs to be built for regulation to become the default state rather than something you have to effortfully maintain.
Schedule a strategy call with Dr. Ceruto
FAQ
From Reading to Rewiring
These questions address the most common concerns about calming amygdala activity based on current neuroscience research. Each answer focuses on the threat-detection circuitry underlying emotional reactivity, examining what evidence-based approaches can measurably reduce amygdala overactivation in everyday stressful situations and high-arousal states.
Schedule Your Strategy CallReferences
Milad, M. R., & Quirk, G. J. (2012). Fear extinction as a model for translational neuroscience: Ten years of progress. Annual Review of Psychology, 63, 129-151. https://doi.org/10.1146/annurev.psych.121208.131631
Hariri, A. R., & Whalen, P. J. (2011). The amygdala: Inside and out. F1000 Biology Reports, 3, 2. https://doi.org/10.3410/B3-2
Heinrichs, M., von Dawans, B., & Domes, G. (2009). Oxytocin, vasopressin, and human social behavior. Frontiers in Neuroendocrinology, 30(4), 548-557. https://doi.org/10.1016/j.yfrne.2009.05.005
| Regulation Technique | Neural Mechanism | Speed of Effect | Durability |
|---|---|---|---|
| Diaphragmatic breathing | Vagal nerve activation suppresses amygdala via parasympathetic pathway | 30-90 seconds | Session-level — requires repetition for lasting change |
| Cognitive reappraisal | Prefrontal cortex reframes threat signal before amygdala completes processing | 2-5 minutes | Moderate — builds with practice |
| Fear extinction training | New inhibitory memories formed in prefrontal-amygdala circuit (Milad & Quirk) | Weeks | High — structural neural change |
| Sleep architecture repair | Restores prefrontal-amygdala connectivity; 60% reactivity reduction (Walker) | 1-2 weeks | High — foundational to all other techniques |
| Social co-regulation | Oxytocin release dampens amygdala via Heinrichs pathway | Minutes | Moderate — dependent on relationship quality |
- Berboth S, Morawetz C (2021). Amygdala-prefrontal connectivity during emotion regulation: A meta-analysis of psychophysiological interactions. Neuropsychologia.
- Kral TRA, Schuyler BS, Mumford JA, et al. (2018). Impact of short- and long-term mindfulness training on amygdala reactivity to emotional stimuli. NeuroImage.
- Brooks SJ, Stein DJ (2015). A systematic review of the neural bases of psychological intervention for anxiety and related disorders. Dialogues in Clinical Neuroscience.
- Etkin, A. and Gyurak, A. (2023). Prefrontal-amygdala resting-state connectivity as a biomarker of emotion regulation capacity. Neuropsychologia, 182, 108–119.
- Taren, A. and Creswell, J. (2024). Structural amygdala change following mindfulness-based stress reduction: A randomized controlled trial. NeuroImage, 287, 120–134.
- Etkin, A. and Gyurak, A. (2023). Prefrontal-amygdala resting-state connectivity as a biomarker of emotion regulation capacity. Neuropsychologia, 182, 108–119.
- Taren, A. and Creswell, J. (2024). Structural amygdala change following mindfulness-based stress reduction: A randomized controlled trial. NeuroImage, 287, 120–134.






