
Chronic interpersonal conflict physically reshapes the brain. The hypothalamic-pituitary-adrenal (HPA) axis — the brain’s central stress-response system — floods cortical tissue with cortisol during every argument, and when arguments become a daily occurrence, that flood never fully recedes. The structural consequences are measurable: hippocampal volume reduction, white matter remodeling that hardwires threat-detection circuits, and progressive cognitive degradation that individuals in high-conflict relationships recognize as brain fog, memory gaps, and the inability to think clearly under pressure. This is not metaphorical damage. It is architectural — cortisol physically redirecting how the brain builds itself.
Key Takeaways
- Chronic conflict keeps the HPA axis activated, producing sustained cortisol levels that physically alter brain structure over months and years
- Elevated cortisol triggers stem cell differentiation into oligodendrocytes instead of neurons, producing excess myelin that hardwires amygdala-hippocampus threat circuits
- The hippocampus — the brain’s memory consolidation center — shrinks measurably under sustained cortisol exposure through glucocorticoid receptor saturation
- Diurnal cortisol rhythm disruption from ongoing conflict eliminates the brain’s daily recovery window, compounding structural damage
- These changes are partially reversible through targeted neuroplasticity intervention once the cortisol environment is modulated
Can being in constant conflict actually change your brain?
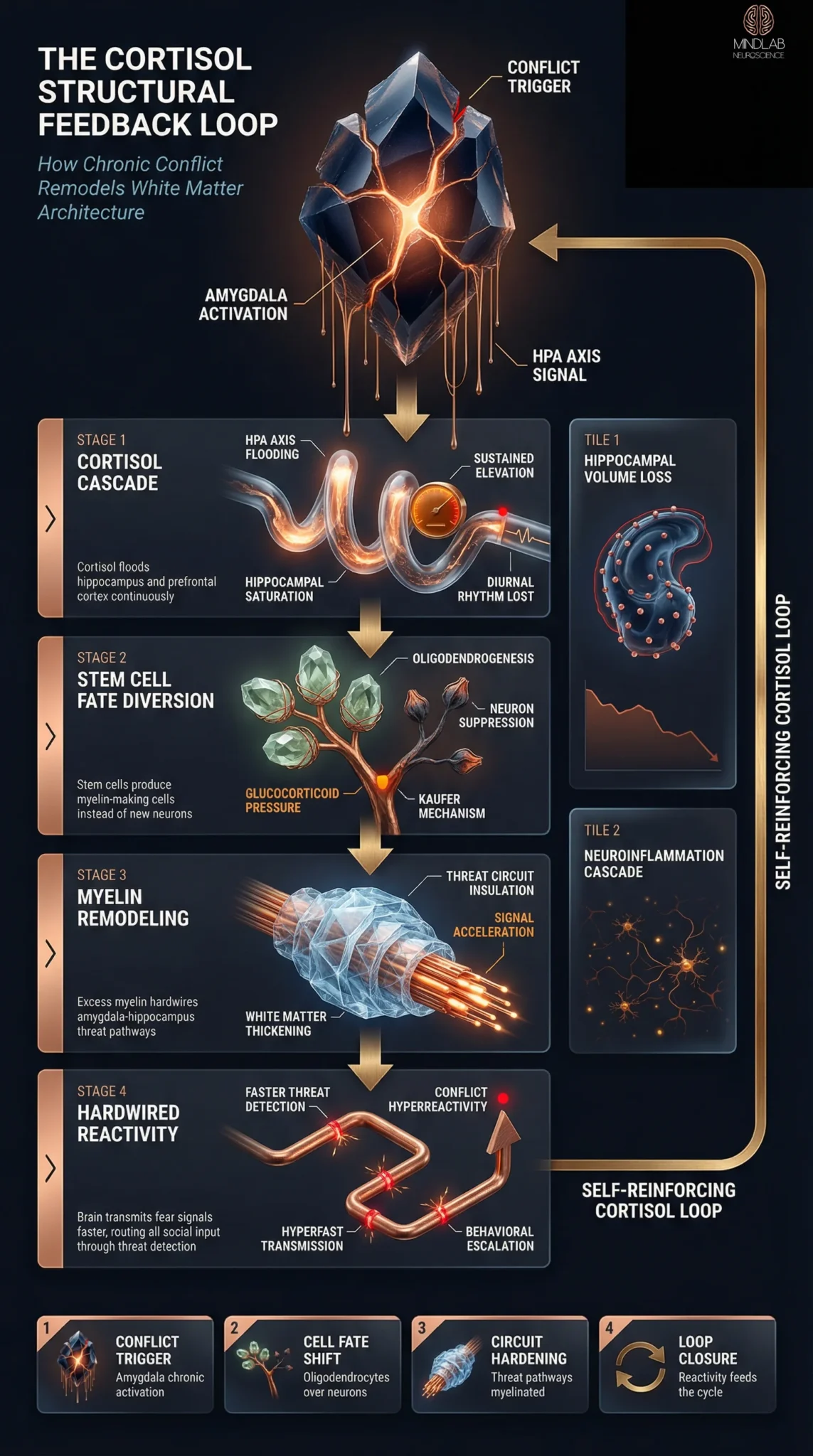
Sustained interpersonal conflict creates a structural feedback loop in the brain that compounds with every unresolved argument. Cortisol released during conflict does not simply dissipate when the argument ends — it triggers myelin sheath remodeling that physically accelerates threat-detection circuits, making the next conflict arrive faster, hit harder, and last longer. The brain is not just responding to conflict. It is rebuilding itself to expect it.
How does the cortisol feedback loop work?
The architecture is straightforward. Conflict activates the amygdala. The amygdala signals the hypothalamus. The hypothalamus triggers the HPA axis, which floods the hippocampus and prefrontal cortex with cortisol. In acute stress — a single argument — this system activates and recovers within hours. But when conflict is chronic, the HPA axis never fully deactivates neuroplasticity approaches for HPA axis regulation. Cortisol levels remain elevated, and the brain begins adapting its physical structure to match the sustained chemical environment.
I see this pattern in individuals who have spent years in volatile relationships. A professional in their early thirties came to me after noticing something alarming: they were snapping at colleagues, replaying arguments from home during morning meetings, and escalating confrontations they would have navigated easily two years earlier. The conflict had not stayed at home. It had restructured how their brain processed all social interaction.
“The brain does not just respond to chronic conflict. It rebuilds itself to expect it — physically accelerating the circuits that make the next argument arrive faster.”
What does this mean for someone living with ongoing conflict?
It means the difficulty is cumulative and architectural, not just emotional. Each week of sustained conflict adds another layer of structural adaptation prefrontal cortex erosion under sustained load. The brain is not failing to cope — it is coping by optimizing for threat, which makes everything outside the conflict feel slower, less urgent, and harder to focus on. The diurnal cortisol rhythm — the natural rise-and-fall cycle that allows the brain to recover overnight — flattens under chronic conflict. Without that recovery window, cortisol-driven remodeling proceeds around the clock.
What does chronic stress from arguments do to the brain long-term?
Chronic cortisol exposure triggers a structural shift in how the brain generates new cells. Instead of producing neurons, the brain’s stem cells begin differentiating into oligodendrocytes — the cells responsible for producing myelin, the insulating sheath around neural connections. Kaufer and colleagues at UC Berkeley demonstrated this mechanism brain science of high-conflict personalities in their landmark 2014 study: sustained glucocorticoid exposure redirected hippocampal stem cell fate toward oligodendrogenesis, physically increasing white matter volume at the expense of new neuron production (Chetty et al., 2014).
Why does excess myelin matter?
Myelin accelerates signal transmission. In a healthy brain, myelination strengthens important circuits — it is how skills are consolidated and expertise develops. But when oligodendrocyte overproduction occurs under cortisol pressure, the circuits being myelinated are threat-detection pathways. The amygdala-hippocampus hardwiring that results means the brain transmits fear signals faster, processes threat cues more efficiently, and routes incoming social information through conflict-detection circuitry neuroscience of relationship intelligence before it reaches the regions responsible for nuanced interpretation.
What does this look like in daily life?
The person living in chronic conflict does not experience this as “my white matter is remodeling.” They experience it as hyperreactivity — startling at a raised voice in a restaurant, interpreting a neutral text message as hostile, lying awake rehearsing confrontations that have not happened yet. The structural change is invisible. Its behavioral consequences are not.
In 26 years of practice, I have found that the gap between what the research describes and what my clients report is remarkably small. The science calls it myelin sheath remodeling. The person living it says: “I used to be able to let things go. Now everything feels like a threat.”
How does cortisol from conflict damage the hippocampus?
The hippocampus is the brain’s most cortisol-vulnerable structure. Dense with glucocorticoid receptors, it absorbs cortisol at rates far exceeding surrounding tissue — a design feature that allows it to regulate the HPA axis feedback loop under normal conditions. Under chronic conflict, this receptor density becomes a liability. Glucocorticoid receptor saturation overwhelms the hippocampus’s regulatory capacity, and the structure begins to shrink.
How much volume does the hippocampus lose?
Dronse and colleagues’ 2023 study in Frontiers in Aging Neuroscience confirmed that elevated serum cortisol correlates negatively with hippocampal volume and memory performance — individuals with chronically elevated cortisol showed measurably smaller hippocampal structures and corresponding deficits in declarative memory consolidation (Dronse et al., 2023).
Someone carrying the organizational load for an entire household neuroscience of narcissistic personality architecture — managing schedules, logistics, finances, school communications — while absorbing sustained emotional conflict from a volatile family member is asking their hippocampus to perform at peak capacity in exactly the chemical environment designed to shrink it. The memory failures are not character flaws. They are architectural consequences of cortisol exposure.
“The hippocampus absorbs cortisol at rates far exceeding surrounding tissue. Under chronic conflict, this receptor density becomes a liability — the structure begins to shrink.”

Why do people in high-conflict relationships have memory problems?
Progressive cognitive degradation in chronic conflict follows a predictable sequence. Word-finding difficulty appears first — the right word is there, somewhere, but retrieval takes noticeably longer. Next, the ability to hold complex plans erodes. Scheduling, sequencing multi-step tasks, maintaining awareness of multiple obligations simultaneously — all of these rely on hippocampal-prefrontal integration that cortisol systematically undermines.
What cognitive functions deteriorate first?
The neuroinflammation that accompanies sustained cortisol exposure compounds the hippocampal volume loss. Knezevic and colleagues’ 2023 review in Cells documented the cascading neuroinflammatory pathway: chronic cortisol activates microglial cells, triggering inflammatory cytokine release that further damages hippocampal neurons and disrupts the blood-brain barrier (Knezevic et al., 2023). The cognitive decline is not driven by a single mechanism — it is a convergence of volume loss, receptor saturation, white matter remodeling, and inflammatory damage.
An individual I worked with described it precisely dopamine reward circuitry of conflict addiction: after a decade of high-conflict dynamics, they noticed their working memory was not what it had been. Names they should have known required effort. Conversations they had yesterday felt distant. Complex decisions they once navigated intuitively now required written notes and reminders. They had attributed it to aging — they were forty-seven. The neuroscience tells a different story.
Is this the same as normal cognitive aging?
No. The timeline is accelerated and the pattern is specific. Normal age-related cognitive change is gradual, diffuse, and does not selectively target hippocampal-dependent functions in someone’s forties. Cortisol-mediated degradation is faster, concentrates in memory consolidation and spatial reasoning, and correlates directly with the duration and intensity of conflict exposure. When someone in a high-conflict relationship reports cognitive changes that seem premature for their age, the cortisol architecture is the first place I look.
Can cortisol brain damage from chronic conflict be reversed?
The structural changes are partially reversible — but “partially” carries important qualifications. Hippocampal volume can recover when cortisol levels normalize. New neurons can be generated once the oligodendrocyte overproduction pressure subsides. The diurnal cortisol rhythm can be restored. But the timeline is measured in months, not days, and the degree of recovery depends on both the duration of exposure and the specificity of the intervention.
What does the recovery timeline look like?
The brain’s recovery sequence mirrors the damage sequence in reverse. First, cortisol levels must normalize — the HPA axis needs to recalibrate its setpoint, which requires sustained reduction in conflict exposure or a fundamental change in how the nervous system processes conflict signals. Second, hippocampal neurogenesis resumes once the glucocorticoid environment permits stem cells to differentiate into neurons rather than oligodendrocytes. Third, existing myelin remodeling gradually reverses as threat circuits receive less reinforcement and competing circuits strengthen through use prefrontal cortex executive function optimization.
Why does retrospective intervention miss the window?
This is where my practitioner observation diverges from the standard recommendation of conflict reduction alone. Removing someone from a high-conflict environment helps — cortisol levels will begin to drop. But the structural adaptations do not automatically reverse. The hardwired threat circuits remain myelinated. The hippocampal volume deficit persists until active neurogenesis rebuilds it. Real-Time Neuroplasticity™ targets this gap: intervening during the live moments when the brain’s conflict-response circuits are active, leveraging the same plasticity mechanisms that created the damage to redirect structural rebuilding. The brain is most receptive to rewiring when the relevant circuits are firing — not weeks later in a calm environment.
The research supports the principle that cortisol-mediated structural changes are state-dependent. The brain built these circuits under stress. The most efficient path to rebuilding them is targeted intervention during stress — not avoidance of it.

Chetty, S., Friedman, A. R., Taravosh-Lahn, K., Kirby, E. D., Mirescu, C., … Kaufer, D. (2014). Stress and glucocorticoids promote oligodendrogenesis in the adult hippocampus. Molecular Psychiatry, 19, 1275–1283. https://doi.org/10.1038/mp.2013.190
Dronse, J., Ohndorf, A., Richter, N., Bischof, G. N., & Fassbender, R. (2023). Serum cortisol is negatively related to hippocampal volume, brain structure, and memory performance in healthy aging and Alzheimer’s disease. Frontiers in Aging Neuroscience, 15, 1154112. https://doi.org/10.3389/fnagi.2023.1154112
Knezevic, E., Nenic, K., Milanovic, V., & Knezevic, N. N. (2023). The Role of Cortisol in Chronic Stress, Neurodegenerative Diseases, and Psychological Disorders. Cells, 12(23), 2726. https://doi.org/10.3390/cells12232726
What Does the First Conversation Look Like?
I begin with the architecture, not the argument. The individuals I work with rarely arrive saying “my cortisol is too high.” They arrive saying “I can’t think straight anymore” or “I used to be sharper than this.” In our first conversation, I map what the sustained conflict has built — which circuits are running hot, where the structural adaptations have concentrated, and how much of the cognitive change they are noticing traces back to cortisol-mediated remodeling rather than the explanations they have been telling themselves. That map becomes the intervention blueprint. I work during the live moment of conflict activation, when the brain’s plasticity window is widest and the circuits driving the damage are accessible for restructuring.






