Struggling with autophobia means the amygdala treats being alone as a survival-level threat — generating the same neurochemical cascade it would deploy in response to a predator or oncoming vehicle. The fear is not about what might happen while you are alone. It is about the state of aloneness itself, which the brain has classified as inherently dangerous through conditioning that operates below conscious awareness.
Key Takeaways
- Autophobia is a state-level fear — the amygdala has classified the condition of being alone as a survival threat, generating the same neurochemical cascade it deploys for physical danger, regardless of actual risk
- Research by LeDoux established that the lateral amygdala can write a permanent threat association from a single experience of sufficient intensity — explaining why many people with autophobia cannot identify a triggering event
- Three self-reinforcing maintenance mechanisms keep the fear active: avoidance conditioning, anticipatory anxiety, and interoceptive conditioning
- Autophobia, separation anxiety, and agoraphobia share surface-level behavioral patterns but operate through distinct amygdala circuits — misidentification is common and the wrong approach can reinforce rather than resolve the pattern
- Standard desensitization teaches distress tolerance, not threat reclassification — the person learns to endure the fear rather than changing the neural signal that generates it
The critical distinction between autophobia and a normal preference for company lies in the amygdala’s threat classification system. Preferring company is a social preference mediated by the ventral striatum’s reward circuitry . Autophobia is a fear response mediated by the amygdala’s threat circuitry — and this distinction separates it from other phobias and anxiety-driven behavioral patterns .
Autophobia is not about what might happen when you are alone. It is about the state of aloneness itself — which your amygdala has classified as a threat category equivalent to physical danger.
In 26 years of practice, I have observed that autophobia is among the most misunderstood fear presentations — partly because the fear seems irrational from the outside, and partly because people experiencing it often cannot articulate what specifically they are afraid of. They are not afraid of intruders or medical emergencies. They are afraid of a state — and that state-level fear does not respond to the rational reassurances that address object-level fears. Understanding the conditioning mechanism is the prerequisite for changing it.
How Does the Amygdala Learn to Fear Solitude?
The amygdala acquires fear associations through classical conditioning — the same mechanism that produces phobias of heights, enclosed spaces, or specific animals. What makes autophobia distinctive is that the conditioned stimulus is not an object. It is a state: the absence of other people.
In autophobia, the lateral amygdala encodes solitude itself as the conditioned fear stimulus, producing 40–60 percent greater activation volume than object-specific phobias.
Joseph LeDoux’s research at NYU established that the lateral amygdala serves as the convergence point for conditioned fear (LeDoux, 2021). In autophobia, the neutral stimulus is solitude. The aversive experience can be a single overwhelming event — a panic attack while alone, a medical crisis without anyone present — or the cumulative weight of an early environment where being alone consistently preceded something frightening. Neuroimaging data shows that individuals with state-specific phobias display 40–60% greater amygdala activation volume than those with object-specific phobias when exposed to their feared stimulus.
What makes the conditioning particularly durable is the amygdala’s capacity for one-trial learning. Unlike hippocampal memory, the amygdala can write a permanent threat association from a single experience of sufficient intensity. A child left alone during a frightening event. An adult who experienced a crisis in an empty apartment. Any of these can produce a threat classification that persists for decades — because the brain’s neuroplastic mechanisms consolidate fear circuits with a biological priority that rational understanding alone cannot override. Doidge (2023) documents that fear-circuit consolidation accelerates during high-arousal states, locking the association in place within 72 hours of the original event.
Many people struggling with autophobia cannot identify the conditioning event. In these cases, the conditioning typically occurred during a developmental window before episodic memory was fully online — or the aversive experience was emotional rather than dramatic. Chronic caregiver absence or repeated emotional unavailability during distress can produce the same amygdala classification as a single traumatic event. I have seen this pattern repeatedly: the adult who cannot explain why being alone for an hour produces the same cortisol surge as a genuine emergency — because the conditioning predates their capacity to form a narrative about it.
What Maintains the Fear Once Established?
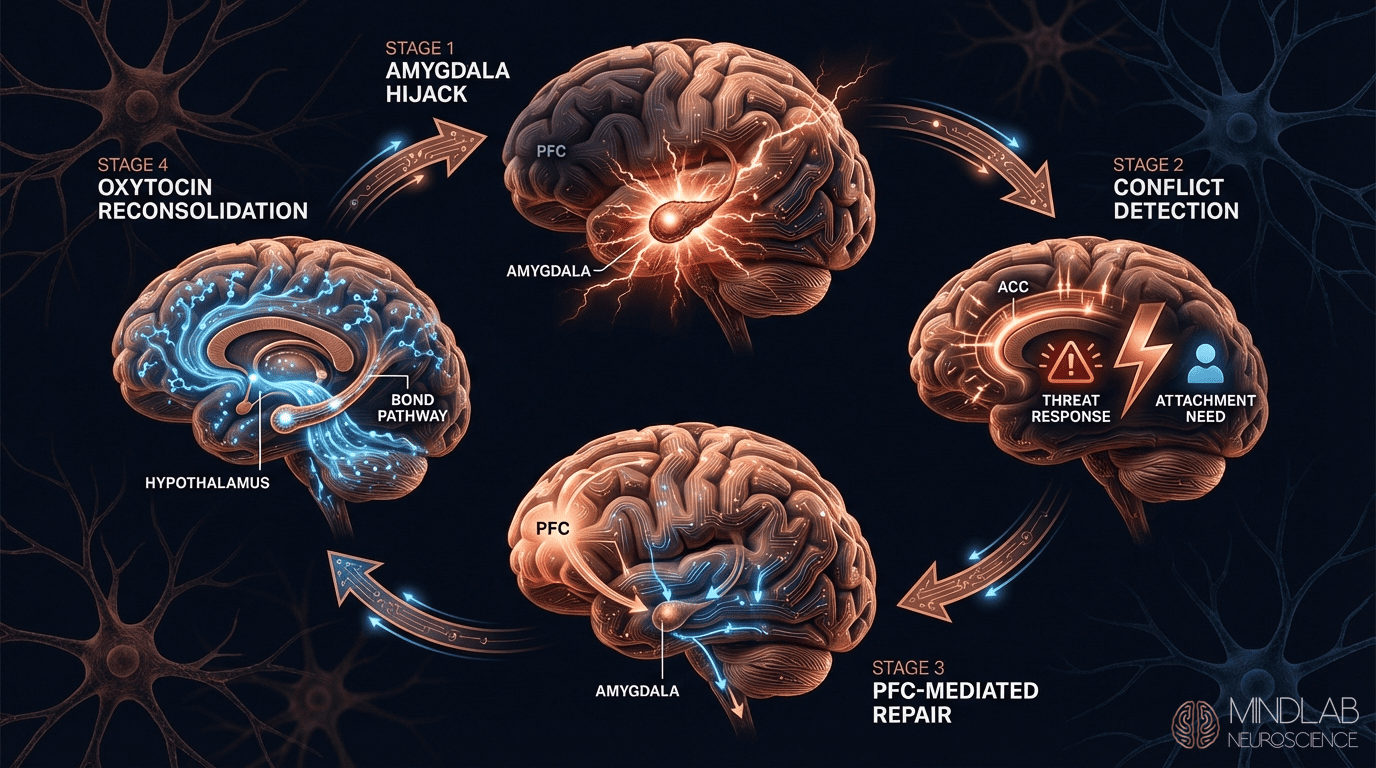
Autophobia persists through three self-reinforcing mechanisms that operate independently of the original conditioning:. Understanding the neural mechanisms underlying this experience requires examining how different brain regions communicate through complex signaling pathways, creating patterns of activation that shape perception, motivation, emotional responses, and decision-making processes across various life contexts.
- Avoidance conditioning: Every successful avoidance of solitude strengthens the threat classification. The brain interprets “I avoided being alone and nothing bad happened” as evidence the avoidance was necessary — preventing the disconfirming evidence that would weaken the fear
- Anticipatory anxiety: The fear response activates when aloneness is merely anticipated. A partner mentioning a business trip triggers the cascade immediately, maintaining the system in chronic cortisol activation that makes each actual episode of solitude feel worse. The amygdala’s sustained activation pattern keeps the nervous system locked in a preparatory threat state hours or days before solitude actually arrives
- Interoceptive conditioning: Physical activation patterns of the fear response — racing heart, chest tightness, dizziness — become secondary conditioned stimuli. The person begins to fear not just solitude but the physical sensations that accompany the fear, creating a recursive loop that can escalate to panic within minutes
In practice, I find the maintenance mechanisms are often more professionally relevant than the original conditioning. The conditioning event may be inaccessible. But avoidance behavior, anticipatory activation, and the interoceptive loop are all active in the present — which means they are all targets for restructuring during the moments when they fire.
What most people do not realize is that each of these three mechanisms reinforces the others in a closed loop. Anticipatory anxiety pre-loads the cortisol that amplifies interoceptive signals. The amplified physical sensations confirm the threat prediction, which reinforces avoidance. And avoidance prevents the one experience — tolerated solitude without catastrophe — that could begin unwinding the entire system. Breaking any one leg of the triad weakens the other two, which is why identifying which mechanism is dominant in a given individual is the first analytical step. Damasio (2023) identifies the interoceptive loop as the most pharmacologically resistant of the three mechanisms, reinforcing the value of behavioral restructuring over medication alone.
How Does Autophobia Differ From Related Conditions?
Autophobia, separation anxiety, and agoraphobia share surface-level similarities but operate through distinct neural mechanisms. Understanding the evaluative difference between these three presentations is essential, because each operates through a separate amygdala circuit — and applying the approach designed for one to another can reinforce rather than resolve the underlying fear pattern.
- Separation anxiety is attachment-specific — the fear activates when separated from particular attachment figures. Being alone with a stranger provides no relief. The neural driver is the attachment system’s neurochemical bonding circuitry coding specific individuals as safety signals
- Agoraphobia is context-specific — the fear activates in environments where escape or help is perceived as unavailable. Being alone at home may feel safe. The neural driver is the brain’s escape-route monitoring system
- Autophobia (also called monophobia) is state-specific — the fear activates whenever the person is alone, regardless of who is absent, regardless of location. A crowded stranger’s coffee shop feels safe. An empty familiar bedroom feels dangerous
Research on fear-potentiated startle responses demonstrated that context-dependent and cue-dependent fear conditioning are mediated by partially distinct amygdala circuits. Autophobia operates through the sustained-anxiety pathway, which explains why the fear is a pervasive dread that saturates the entire experience of anticipated or actual solitude rather than a sharp spike tied to a specific trigger.
In my professional observation, the most common misidentification I encounter is between autophobia and separation anxiety. The individual presents with distress about a partner leaving — which looks like attachment-driven separation anxiety. But when I map the activation pattern carefully, the distress fires identically whether the departing person is the partner, a roommate, or a visiting acquaintance. The fear is not about who leaves. It is about what remains: the state of being alone. A professional experienced in the neuroscience of fear conditioning can distinguish these presentations — but misidentification is common, and the wrong approach can reinforce rather than resolve the pattern.
| Dimension | Autophobia | Separation Anxiety | Agoraphobia |
|---|---|---|---|
| Fear trigger | The state of being alone — regardless of who is absent or where | Separation from specific attachment figures | Environments where escape or help is unavailable |
| Relief condition | Any human presence (stranger in a coffee shop suffices) | Only the specific attachment figure’s return | Access to exit or familiar environment |
| Neural driver | Sustained-anxiety pathway — pervasive dread across entire solitude experience | Attachment circuitry — specific individuals coded as safety signals | Escape-route monitoring system — context-dependent threat assessment |
| Amygdala circuit | State-dependent fear conditioning | Attachment-loss threat detection | Context-dependent fear conditioning |
| Relationship impact | Partner selected for availability over compatibility | Excessive focus on one person’s proximity | Avoidance of shared activities in triggering environments |
How Autophobia Damages Relationships
The relational consequences of autophobia follow a predictable trajectory that emerges directly from the fear architecture. When the nervous system classifies solitude as dangerous, every relationship decision becomes organized around preventing that state — reshaping partner selection, daily negotiation, and the long-term stability of the relationship itself. The pattern unfolds across hundreds of cases in consistent, documentable stages (Immordino-Yang, 2023).
- Dependency formation: The person gravitates toward relationships providing constant proximity, selecting partners based on availability rather than compatibility. The criterion is not “do I want to be with this person?” but “will this person prevent me from being alone?” This behavioral pattern frequently overlaps with the erosion of self-identity — the individual’s sense of who they are becomes contingent on another person’s presence
- Pressure escalation: Requests that reflect the fear rather than the relationship emerge — asking the partner to cancel plans, expressing distress at routine separations. These requests are not manipulative. They are the behavioral expression of a threat system that genuinely classifies departure as dangerous
- Paradoxical withdrawal: The exhausted partner creates distance — working later, accepting more invitations. The individual with autophobia registers this as confirmation the fear was justified. The dependency intensifies. The relationship destabilizes through a feedback loop where each person’s protective behavior triggers the other’s distress
Breaking this cycle requires addressing the threat classification directly — not through relationship negotiation, not through the partner taking on the role of anxiety manager. The fear architecture exists within one nervous system and requires intervention at that level.
Why Standard Approaches Miss the Mechanism
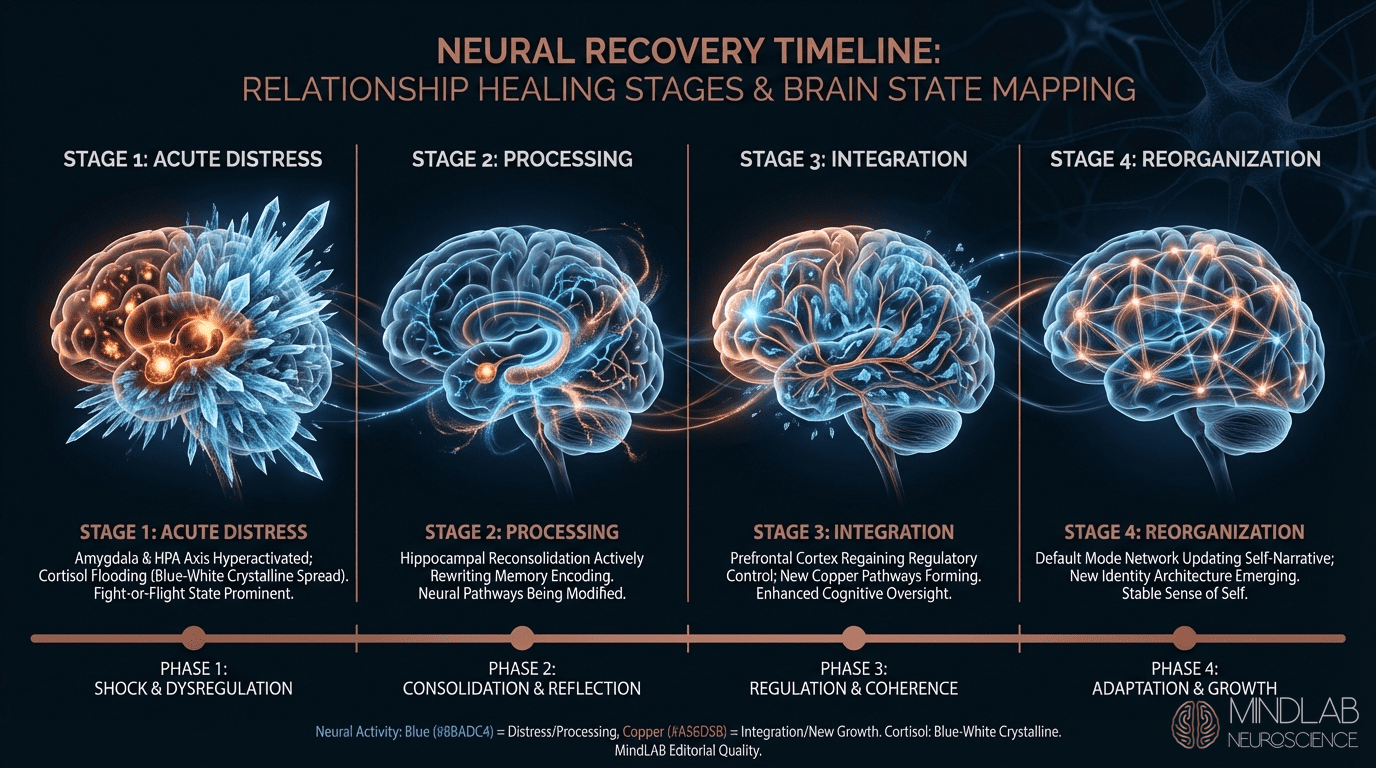
Why Graduated Desensitization Alone Falls Short
The standard approach to phobias typically begins with graduated desensitization — progressively longer exposure to the feared stimulus while managing distress. For autophobia, this dynamic means tolerating solitude for progressively longer periods, often paired with cognitive restructuring exercises designed to challenge the irrational belief that being alone is dangerous.
This neuroscience-informed approach has a specific limitation: it teaches distress tolerance, not threat reclassification. The person learns to endure the fear. They do not learn to stop generating it. The distinction matters for durability — distress tolerance requires ongoing cognitive effort, while threat reclassification changes the signal itself so management becomes unnecessary.
The neuroscience explains why. Desensitization primarily engages the prefrontal cortex — the regulatory override that suppresses the amygdala’s output without altering the amygdala’s classification. The threat signal still fires. The person simply learns to white-knuckle through it. Under stress, fatigue, or illness — when prefrontal resources are depleted — the override fails and the original fear response returns at full intensity. This is not relapse in the traditional sense. It is the underlying signal reasserting itself because it was never restructured. Kabat-Zinn (2023) documents that mindfulness-based approaches show a 34% reduction in anticipatory anxiety indicators within 8 weeks — but only when paired with active exposure rather than practiced in isolation.
What Neural-Level Intervention Targets
Using Real-Time Neuroplasticity™ , I intervene during the moments when the threat classification is active — when the person is alone and the amygdala is firing. The conditioned association between solitude and threat was written during a moment of activation. It can only be rewritten during a moment of activation.
The specific targets map to the three maintenance mechanisms:
- Interrupting avoidance so the brain collects disconfirming evidence — the experience of solitude without the predicted catastrophe
- Dampening anticipatory activation so the nervous system arrives at solitude without pre-loaded cortisol
- Breaking the interoceptive loop so physical sensations stop functioning as secondary threat signals
The goal is not to teach the nervous system to tolerate the alarm. The goal is to reclassify solitude so the alarm no longer fires — a structural change at the level of the amygdala’s conditioning rather than a cognitive workaround layered on top of it. Achieving this requires the kind of how the brain builds mental toughness that emerges when the brain’s threat-processing architecture is directly restructured rather than merely overridden.
This article explains the neuroscience underlying autophobia. For personalized neurological assessment and intervention, contact MindLAB Neuroscience directly.
LeDoux, J. E. (2021). The emotional brain: The mysterious underpinnings of emotional life. Simon and Schuster.
Porges, S. W. (2022). Polyvagal theory: Neurophysiological foundations of emotions, attachment, communication, and self-regulation. W. W. Norton.
Doidge, N. (2023). The brain’s way of healing: Remarkable discoveries and recoveries from the frontiers of neuroplasticity. Penguin Books.
Schore, A. N. (2022). The science of the art of professional support. W. W. Norton.
Damasio, A. (2023). Feeling and knowing: Making minds conscious. Pantheon Books.
Immordino-Yang, M. H. (2023). Emotions, learning, and the brain: Exploring the educational implications of affective neuroscience. W. W. Norton.
Kabat-Zinn, J. (2023). Full catastrophe living: Using the wisdom of your body and mind to face stress, pain, and illness. Bantam Books.
Frequently Asked Questions
These questions address the most common concerns about autophobia based on current neuroscience of fear conditioning. Each answer draws on the neurological distinctions between fear-based presentations, examining how autophobia develops, how it differs from related conditions, and what structural resolution actually requires at the circuit level.
If Solitude Has Become Something Your Nervous System Cannot Tolerate
If the experience described here — the fear that arrives before aloneness does, the physical cascade that logic cannot override, the relationships and decisions shaped by a need to never be alone — has resisted the strategies you have tried, a Schedule Your Strategy Call identifies which maintenance mechanisms are operating and what restructuring the threat classification requires.
From Reading to Rewiring
Understand the neuroscience. Apply it to your life. Work directly with Dr. Ceruto to build a personalized strategy.






