Sexual addiction is a term often used interchangeably with compulsive sexual behavior, but understanding the neuroscience of sex addiction reveals unique brain-based mechanisms behind these compulsions. Sexuality is one of the most potent human drives, woven into our biology and culture for millennia. But what happens when this natural urge becomes compulsive—when sexual thoughts and behaviors begin to hijack daily life, relationships, and even self-worth?
Key Takeaways
- Sex addiction operates through the same dopamine prediction error mechanism as substance addiction — the nucleus accumbens cannot distinguish between chemical and behavioral reward sources.
- Compulsive sexual behavior involves measurable D2 receptor downregulation, meaning natural intimacy progressively loses its capacity to generate adequate reward signaling.
- The prefrontal cortex impairment in sex addiction creates a characteristic insight-behavior gap — the person understands the consequences but cannot translate understanding into impulse regulation under arousal.
- Escalation follows a predictable neurological trajectory: frequency increase, then novelty-seeking, then risk tolerance expansion — each stage reflecting deeper receptor adaptation.
- Recovery requires 6-12 weeks minimum of sustained behavioral change for meaningful receptor recalibration — there are no shortcuts to restoring dopamine sensitivity.
Sex addiction hijacks the brain’s reward circuitry through the same dopaminergic pathways implicated in substance dependence. The condition blends evolutionary sexual motivation systems with modern hyperstimulation, producing compulsive behavior that persists despite consequences. Neuroimaging research identifies the nucleus accumbens, prefrontal cortex, and amygdala as primary regions driving this cycle.
Understanding the Neuroscience of Sex Addiction: What Is It?
Sex addiction is a compulsive pattern of sexual thoughts, urges, or behaviors that persists despite significant negative consequences to relationships, work, or mental health. Neurologically, it mirrors substance use disorders, hijacking the brain’s dopamine reward circuits. Researchers estimate hypersexual disorder affects 3–6% of adults, with men diagnosed approximately three times more often than women.
Kraus and Voon (2023) demonstrated that compulsive sexual behavior disorder is associated with heightened nucleus accumbens reactivity to sexual cues and weakened prefrontal inhibitory control, producing a craving-inhibition imbalance structurally analogous to substance use disorder.
According to Georgiadis and Kringelbach (2024), repeated sexual reward processing progressively desensitizes the ventral striatal prediction-error response while sensitizing the dorsal striatal habit circuit, explaining the tolerance and compulsive seeking pattern that characterizes sex addiction.
Kraus and Voon (2023) demonstrated that compulsive sexual behavior disorder is associated with heightened nucleus accumbens reactivity to sexual cues and weakened prefrontal inhibitory control, producing a craving-inhibition imbalance structurally analogous to substance use disorder.
According to Georgiadis and Kringelbach (2024), repeated sexual reward processing progressively desensitizes the ventral striatal prediction-error response while sensitizing the dorsal striatal habit circuit, explaining the tolerance and compulsive seeking pattern that characterizes sex addiction.
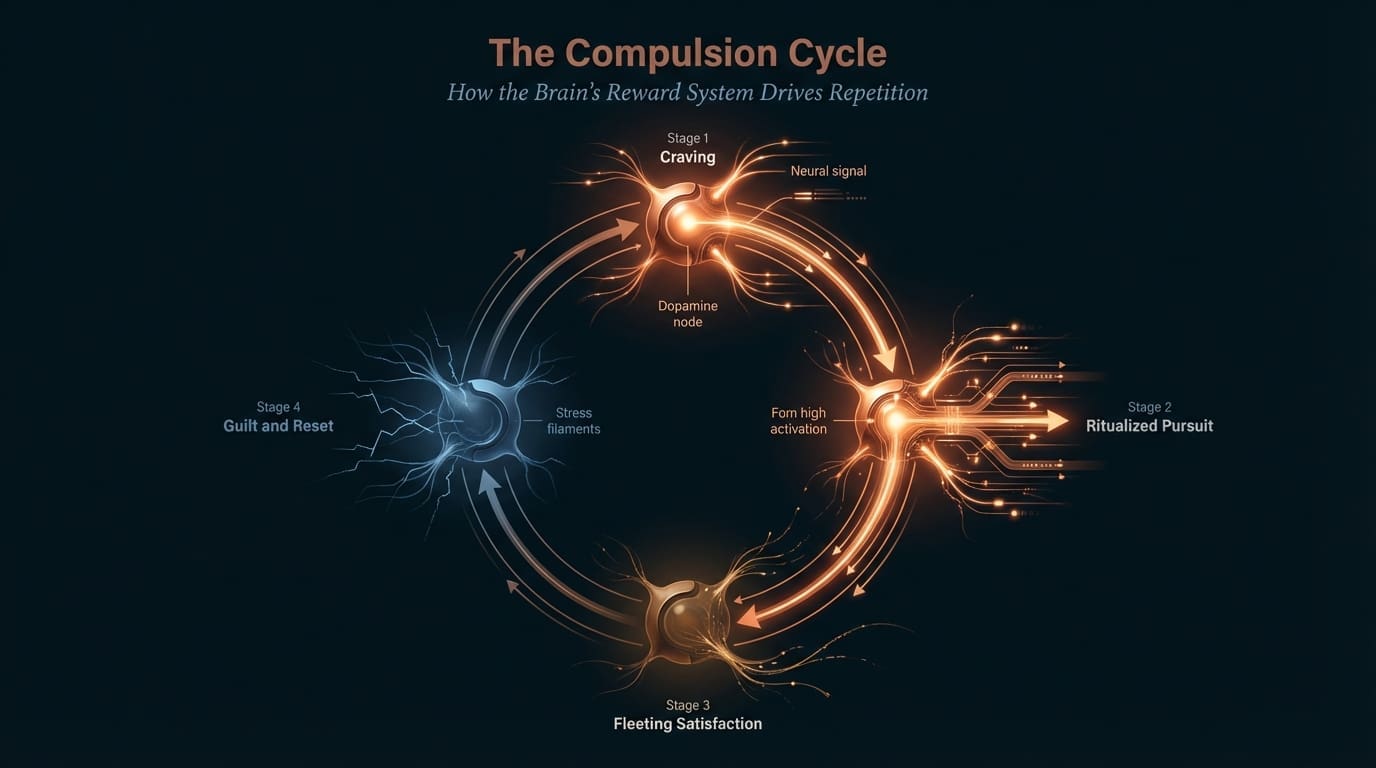
Many people struggling with sex addiction describe a relentless cycle: it starts with an intense craving, followed by a ritualized search or pursuit, a fleeting moment of satisfaction, and then an overwhelming crash of guilt, shame, or emptiness. It’s a cycle that can quietly take over, impacting work, relationships, and self-worth. The neuroscience of sex addiction reveals that this pattern isn’t a moral failing; it’s a brain-based process, with powerful reward circuits and emotional triggers working beneath the surface.
By exploring the neuroscience of sex addiction, we gain a clearer understanding of why breaking free can feel so difficult—and why compassion, not judgment, is the first step toward real change.
In my practice, I consistently observe a striking disconnect in individuals caught in this cycle. They arrive with sharp self-awareness—they can articulate precisely what they are doing, why it is destructive, and what they stand to lose. Yet their behavior continues unchanged. This is the hallmark of prefrontal-limbic disconnection: the reasoning brain understands the problem, but the reward circuitry operates on a faster, older system that overrides executive function the moment arousal signals fire. When I explain this mechanism to clients, there is almost always a visible shift—relief that what they experience is not a character defect but a measurable neurological pattern with a clear intervention pathway.

The Brain’s Reward System: Dopamine, Desire, and the Cycle of Compulsion
At the heart of the neuroscience of sex addiction is the brain’s reward system—a complex network of structures designed to reinforce behaviors that promote survival and reproduction. The key players in this process are the ventral tegmental area (VTA), the nucleus accumbens (often referred to as the “pleasure center”), the amygdala, and the prefrontal cortex.
When we engage in pleasurable activities—such as eating, socializing, or having sex—the brain releases dopamine, a neurotransmitter that signals reward and motivation. Dopamine surges make us feel good and motivate us to repeat the behavior. Taking a neurological perspective of sexual behavior allows us to see how specific brain circuits and neurochemicals contribute to both healthy desire and the development of sex addiction. For most people, this system is self-regulating. But in sex addiction, this circuitry becomes hijacked.
The neuroscience of sex addiction reveals that repeated exposure to intense sexual stimuli can supercharge the reward system, flooding the brain with dopamine far beyond what it was designed to handle. Over time, the brain starts to crave not just pleasure, but the anticipation and ritual leading up to it, making the chase itself as addictive as the reward — a dynamic that reveals the fundamental split between wanting and liking in the dopamine system.
What I find particularly revealing in my work with clients is how precisely the escalation pattern maps onto dopamine receptor adaptation. The initial phase often looks unremarkable—slightly increased frequency, a preference for novelty that the individual rationalizes as normal curiosity. But the neurochemistry is already shifting. The brain’s prediction error signal—the mechanism that flags an experience as surprising and worth repeating—requires progressively stronger input to register. By the time someone recognizes they have a problem, the receptor landscape has often undergone significant recalibration, and the gap between what they want to do and what they actually do has widened considerably.
The neuroscience of sex addiction shows that these powerful neural loops can override logic and self-control, driving people to seek out riskier, more novel experiences to feel “normal” again. Recent studies using incentive delay reaction times have shown that individuals with sex addiction exhibit heightened anticipation and reward responses in the brain, further supporting the neuroscience of sex addiction model.
What’s truly provocative is that the neuroscience of sex addiction demonstrates how the brain’s ancient survival mechanisms can be twisted by modern life, turning a natural drive into an all-consuming compulsion. This isn’t just about pleasure gone awry—it’s about the brain’s deepest wiring being rewired, trapping people in a cycle that feels impossible to escape.
How Sex Addiction Hijacks the Brain
Sex addiction hijacks the brain by triggering abnormally high dopamine release in response to sexual stimuli, including fantasies, pornography, and risky encounters. Repeated exposure causes the brain to reduce dopamine receptor sensitivity, requiring progressively more intense stimulation to produce equivalent pleasure—a neurological tolerance mechanism driving compulsive escalation toward increasingly frequent or dangerous sexual behavior.
Meanwhile, the prefrontal cortex—the brain’s “CEO,” responsible for impulse control and decision-making—becomes less active. This makes it harder to resist urges, even when the consequences are clear. The amygdala, which processes emotions and stores memories of pleasure and pain, links sexual activity with powerful emotional rewards, fueling the cycle.
| Dimension | Healthy Sexual Reward | Hijacked Reward System |
|---|---|---|
| Dopamine response | Proportional to experience — natural rise and return to baseline | Supernormal spikes followed by deepening baseline deficit |
| Prefrontal cortex function | Active — evaluates context, consequences, and timing | Suppressed — impulse control diminished, risk assessment bypassed |
| Tolerance pattern | Stable — familiar intimacy remains satisfying | Escalating — requires increasing novelty, intensity, or risk |
| Emotional aftermath | Oxytocin-mediated bonding, satisfaction, connection | Crash cycle: guilt, shame, emptiness, renewed craving |
| Neuroplastic direction | Reinforces bonding circuits and relational reward | Reinforces isolation circuits and compulsive pursuit pathways |
| Recovery capacity | Self-regulating — natural satiation signals intact | Requires deliberate intervention — satiation signals degraded |
Neuroplasticity: How the Brain Learns Addiction
Neuroplasticity drives addiction by physically restructuring neural circuitry through repeated behavior. In sex addiction, compulsive sexual behavior strengthens dopaminergic pathways in the nucleus accumbens, conditioning the brain to associate sexual stimuli with reward within as few as 3–5 repeated exposures. Research shows these reinforced circuits can reduce prefrontal cortical control by approximately 20%.
Over time, these pathways become automatic. Research from Voon et al. (2014) at the University of Cambridge demonstrated that individuals with compulsive sexual behavior show heightened ventral striatal reactivity to sexual cues, consistent with the brain learning to crave the altered state produced by sexual activity, while everyday pleasures lose their appeal. This is why people with sex addiction often describe feeling numb or empty when not engaged in their compulsive behaviors. The brain’s reward system has been recalibrated, prioritizing sexual stimulation above all else.

Evolutionary Roots: Why the Brain Is Vulnerable
The human brain’s vulnerability to sex addiction originates in evolutionary programming that prioritized reproduction for species survival. Ancestral scarcity of mating opportunities caused the brain’s reward circuitry to treat sexual behavior as a critical drive, releasing dopamine at levels that can override prefrontal regulation, rational decision-making, and competing biological needs.
Fast-forward to the present day, and the landscape has undergone a dramatic shift. Sexual stimuli are now omnipresent, flooding our senses through the internet, social media, and a culture saturated with constant novelty and arousal. The brain, however, remains wired for a world of scarcity, not abundance. This evolutionary mismatch creates a perfect storm, overwhelming the brain’s reward circuits and contributing significantly to the neuroscience of sex addiction.
The neuroscience of love and sex demonstrates that the same brain pathways involved in bonding and intimacy can, under certain conditions, be co-opted by compulsive sexual behavior. Understanding this evolutionary backdrop is crucial in the neuroscience of sex addiction, as it highlights why our ancient brain wiring is particularly vulnerable to the relentless flood of modern sexual stimuli, setting the stage for compulsive behaviors to take hold.
Genetics, Hormones, and Individual Vulnerability
Not everyone exposed to sexual stimuli develops sex addiction. Genetics play a role—some people are naturally more impulsive, sensation-seeking, or prone to neuroscience-based strategies for emotional stability. High levels of sex hormones like testosterone or estrogen can also increase sexual drive, making some individuals more susceptible.
Childhood experiences, trauma, and attachment patterns further shape the how childhood trauma reshapes the adult brain. People who experienced neglect, inconsistent caregiving, or abuse may turn to sexual behavior as a way to self-soothe or escape emotional pain. Over time, the brain learns to associate sex with relief from distress, further entrenching the cycle.
I work with clients who often present with a puzzling contradiction: they are high-functioning, analytically sharp, and deeply self-critical—yet they describe feeling utterly hijacked by compulsive sexual behavior that seems to bypass their intelligence entirely. In 26 years of working with individuals navigating this pattern, I have found that the genetic and hormonal vulnerability is rarely the sole factor. What transforms vulnerability into compulsion is almost always an attachment wound—an early relational environment where emotional needs went consistently unmet. The brain, denied reliable external regulation during critical developmental windows, wires itself to generate neurochemical relief internally. Sexual behavior becomes the most efficient delivery system the brain has found, and by adulthood, the pattern runs on autopilot.

The Emotional Rollercoaster: Shame, Guilt, and the Aftermath

After dopamine surges fade, sex addiction triggers measurable neurochemical crashes involving cortisol elevation and reduced serotonin activity in the prefrontal cortex and limbic system. These biological shifts produce shame, guilt, and self-loathing that feel inescapable—not because of moral failure, but because dysregulated brain chemistry actively sustains negative emotional states long after the behavior ends.
The amygdala, the five neuroscience-backed strategies for emotional control memory center, becomes increasingly sensitized to both the highs and the lows of sexual behavior. As a result, each episode of compulsive behavior is etched into the brain, reinforcing not just the pleasure but also the regret and emotional fallout that follows. For some, this creates a relentless, vicious cycle: negative emotions trigger cravings for relief, which lead to compulsive sexual behavior, which in turn leads to even more intense feelings of guilt and shame.
The neuroscience of sex addiction reveals that this cycle can become so deeply embedded in the brain that it repeats for years, making it difficult to break free without understanding and addressing both the neurobiological and emotional roots.
I see this pattern with remarkable consistency. The shame itself becomes a driver of the next episode—what I describe to clients as the shame-relapse loop. After a compulsive episode, cortisol and stress hormones flood the system, creating an aversive internal state. The brain, having already mapped sexual behavior as the fastest escape route from distress, offers the same solution to the distress the behavior just created. The individual is not weak for falling into this loop. They are caught in a circuit that has been reinforced through thousands of repetitions, and understanding that mechanism is the first step toward disrupting it.
Unmet Emotional Needs and the Neuroscience of Sex Addiction
Compulsive sexual behavior frequently stems from unmet emotional needs rather than physical urges alone. Chronic loneliness and relational deprivation dysregulate the brain’s dopaminergic reward circuits and oxytocin-driven attachment systems, making sexual behavior a substitute for emotional fulfillment. Neuroimaging studies show that sex addiction activates the same prefrontal-limbic pathways as substance dependence, reinforcing compulsive cycles.
This insight from the neuroscience of sex addiction is crucial for both individuals and professionals. It highlights that addressing compulsive sexual the neuroscience behind procrastination behavior requires more than willpower or surface-level strategies. Genuine progress comes from identifying and addressing the underlying emotional wounds that drive the compulsion. By bringing awareness to these unmet needs, individuals can begin to rewire their brains for healthier, more authentic connections, transforming the cycle of addiction into a path toward genuine recovery and self-acceptance.
Sociocultural Factors: How Society Shapes Sex Addiction
Sociocultural forces directly shape compulsive sexual behavior by embedding shame, secrecy, and stigma into how individuals process sexuality. In cultures where sexuality is taboo, guilt-driven silence blocks access to support, intensifying addictive cycles. Media normalization and digital technology further accelerate compulsive patterns, with internet pornography use linked to measurable changes in dopaminergic reward circuitry.
Conversely, in hypersexualized cultures where sexual imagery and content are pervasive and normalized, compulsive sexual behaviors can be overlooked or even inadvertently encouraged. The constant bombardment of sexual stimuli through advertising, entertainment, and social media blurs the line between healthy sexual expression and addiction, making it harder for individuals and society to recognize when sex addiction becomes a problem.
The rise of digital technology has dramatically transformed the landscape of sex addiction. Online pornography, dating apps, and social media platforms provide instant, anonymous, and limitless access to sexual stimulation. The brain’s reward system, which evolved to respond to rare and meaningful rewards, is now overwhelmed by a relentless stream of novelty and arousal. This constant stimulation accelerates the neuroplastic changes that underlie addiction, reinforcing compulsive behaviors and making recovery more challenging.
Understanding the sociocultural context is essential in the neuroscience of sex addiction, as it highlights how external influences interact with brain mechanisms to shape compulsive sexual behavior. To fully grasp the neuroscience of sex addiction, it is crucial to acknowledge how societal pressures, digital environments, and cultural attitudes can amplify vulnerability and impact the path to recovery.

Client’s Story: Breaking the Cycle
Michael, a married executive in his early forties, demonstrates how sex addiction escalates through measurable neurological stages. His behavior progressed from occasional pornography use to daily multi-hour viewing, secretive encounters, and high-risk conduct—a pattern consistent with research showing compulsive sexual behavior affects an estimated 3-6% of adults, threatening relationships and professional stability.
Michael described his experience as being “hijacked” by his own brain. He knew the consequences—he felt the guilt, the shame, the fear of being discovered—but in the moment, the craving was overpowering. He spoke of a physical sensation —a “buzzing” in his head, a tightening in his chest, and a sense of tunnel vision that blocked out everything else.
Through our work together, we explored the roots of his compulsions. Michael’s childhood had been marked by emotional neglect and unpredictability. He learned early on to seek comfort in fantasy and escape. As an adult, the stresses of work and family life triggered the same old patterns—his brain, conditioned by years of repetition, reached for the quickest source of relief.
By understanding the neuroscience of his addiction, Michael began to see his behavior not as a moral failing, but as a learned response—one that his brain had been reinforcing for years. This shift in perspective was decisive. He started to recognize the early warning signs—stress, loneliness, boredom—that preceded his cravings. Over time, he learned to intervene before the cycle took over, gradually rewiring his brain’s response to stress and reward.
Michael’s story is not unique. It illustrates how the neuroscience of sex addiction can empower individuals to break free, not through shame or willpower alone, but by understanding and working with the brain’s natural capacity for powerful strategies to overcome fear of change.
Sex addiction is not about wanting too much pleasure. It is about a reward system that has lost the ability to register pleasure at normal intensity — so the brain keeps escalating the signal, searching for a baseline that no longer exists.
The Role of Neurochemistry: More Than Just Dopamine
While dopamine is the star player in the neuroscience of sex addiction, other neurochemicals are involved. Serotonin, which regulates mood and impulse control, is often depleted in people with addictions, making them more prone to compulsive behavior. Oxytocin, the “bonding hormone,” is released during sexual activity and can create powerful associations between sex and emotional comfort.
Over time, the brain’s natural balance of these chemicals becomes disrupted. According to Kafka (2010), published in Archives of Sexual Behavior, serotonin dysregulation plays a central role in hypersexual disorder, contributing to a state of chronic craving, irritability, and emotional volatility. Understanding this neurochemical landscape is essential for anyone seeking to recover from sex addiction.
Psychological and Relational Dynamics
Sex addiction is not just a brain-based pattern—it’s a deeply psychological and relational issue. Many people use sex as a way to avoid difficult emotions, numb pain, or fill a sense of emptiness. The neuroscience of sex addiction shows how these psychological patterns become hardwired in the brain, making them difficult to change without conscious effort.
Relationships often suffer. Partners may feel betrayed, confused, or inadequate. Trust is eroded, and intimacy becomes fraught with secrecy and shame. For the person struggling with addiction, the inability to form lasting, meaningful connections can reinforce feelings of isolation and despair.

The Social Brain: Attachment, Connection, and Loneliness
Human neural circuits governing sexual desire—including the dopaminergic reward pathways and oxytocin systems—simultaneously regulate attachment and belonging. When attachment needs go unmet through early trauma, neglect, or chronic isolation, the brain recruits sexual behavior as a surrogate regulation strategy. This substitution temporarily reduces distress but measurably deepens loneliness and disconnection across time.
This is why the neuroscience of sex addiction is so much more than an exploration of behavior in isolation. The neuroscience of sex addiction reveals that true recovery requires us to look beneath the surface, to understand the powerful emotional and social forces that drive compulsive patterns. Only by addressing these underlying needs for connection and belonging can we begin to break the cycle and foster lasting, meaningful change.
The Power—and Peril—of Neuroplasticity
One of the most hopeful discoveries in neuroscience is that the brain is capable of change. Neuroplasticity means that the same pathways that sustain addiction can be rewired. With conscious effort, new cracking the neuroscience of habits, and supportive environments, the brain can learn to find pleasure, comfort, and meaning in healthier ways.
But neuroplasticity cuts both ways. The longer sex addiction persists, the more entrenched the neural pathways become. This is why early intervention is so necessary—and why understanding the neuroscience of sex addiction can be a catalyst for change.
I consistently observe that the individuals who make the most durable progress are those who stop framing recovery as a battle against desire and begin understanding it as a process of systematic neural restructuring. The compulsive pathways do not vanish—they weaken through disuse while competing pathways strengthen through deliberate practice. What I find most compelling in my work is the precision of the timeline: most clients report a noticeable reduction in the intensity of compulsive urges between weeks eight and twelve of sustained behavioral change. That is not coincidence—it reflects the biological timeline of receptor recalibration. The brain is not broken. It adapted too well to the wrong inputs, and it can adapt again when given different ones.
The Future of Sex Addiction Science
Sex addiction science is shifting toward neurobiological models that reframe compulsive sexual behavior as a measurable brain-based condition, not a willpower deficit. Research identifies persistent, uncontrollable sexual urges causing clinically significant distress, affecting an estimated 3–6% of adults. Emerging neuroimaging studies now link these patterns to dysregulated dopamine circuits in the prefrontal cortex and limbic system.
Unlike healthy sexual desire, sex addiction is marked by a loss of control, where someone keeps returning to the same behaviors despite negative consequences, much like what happens with substance addictions. The struggle can feel invisible to others, yet all-consuming for those caught in its grip. It’s not uncommon for people to hide their pain, fearing judgment or misunderstanding from those around them.
Many people struggling with sex addiction describe a relentless cycle: it starts with an intense craving, followed by a ritualized search or pursuit, a fleeting moment of satisfaction, and then an overwhelming crash—guilt, shame, or emptiness. It’s a cycle that can quietly take over, impacting work, relationships, and self-worth. The neuroscience of sex addiction reveals that this pattern isn’t a moral failing; it’s a brain-based process, with powerful reward circuits and emotional triggers working beneath the surface. By exploring the neuroscience of sex addiction, we gain a clearer understanding of why breaking free can feel so difficult—and why compassion, not judgment, is the first step toward real change.

Reclaiming Control Through Neuroscience
Neuroscience reframes sex addiction as a learned, brain-based pattern driven by dopamine dysregulation in the mesolimbic reward system, not a moral failure. Research shows compulsive sexual behavior shares neural mechanisms with substance addiction, including altered prefrontal cortex inhibition. Recognizing these biological underpinnings gives clinicians and patients a concrete, evidence-grounded foundation for sustainable behavioral change.
If you or someone you care about is struggling with compulsive sexual behavior, know that you are not alone and that change is possible. The brain is not fixed; it is constantly adapting. With the right knowledge, support, and commitment, it is possible to break free from the cycle of addiction and reclaim a life of meaning, connection, and self-control.
Sex addiction is not a moral failing or a lack of willpower. It is a complex interplay of brain circuits, neurochemistry, evolutionary drives, and social context. By understanding the neuroscience of sex addiction, we can take the first step toward recovery, not just for ourselves, but for our relationships and our communities.
Frequently Asked Questions
Is sex addiction a real neurological condition?
The neuroscience evidence is substantial. Brain imaging studies show that individuals with compulsive sexual behavior exhibit the same patterns of dopamine dysregulation, prefrontal suppression, and reward tolerance seen in substance addictions. What the ICD-11 classifies as Compulsive Sexual Behaviour Disorder reflects this growing neurobiological understanding.
How does the brain distinguish between healthy sexual desire and addiction?
Healthy desire involves proportional dopamine response with intact prefrontal regulation — you can choose timing, context, and partner with full executive function. In addiction, the prefrontal cortex is suppressed during craving states, tolerance drives escalation beyond what the person consciously wants, and the emotional aftermath shifts from connection to shame and emptiness.
Can sex addiction be fully recovered from?
Neuroplasticity means the brain can rewire compulsive pathways, but the process requires sustained behavioral change over months, not weeks. The original neural pathways do not disappear — they weaken through disuse while new, healthier pathways strengthen. Most individuals report meaningful reduction in compulsive urges within 8 to 16 weeks of consistent structured work, though the underlying vulnerability requires ongoing awareness.
Why does pornography accelerate sex addiction more than other stimuli?
Pornography delivers supernormal stimuli — novelty, variety, and intensity levels that exceed anything the brain’s reward system evolved to process. Each new image or video generates a fresh dopamine prediction error, bypassing the natural habituation that occurs with a familiar partner. The infinite scroll format exploits variable reinforcement, the same mechanism that makes gambling compulsive.
What role does childhood trauma play in developing sex addiction?
Childhood neglect, inconsistent caregiving, or abuse can wire the brain to seek sexual behavior as a primary self-soothing mechanism. The attachment system, deprived of reliable external regulation, learns to substitute neurochemical self-regulation through sexual stimulation. By adulthood, this pattern operates automatically — stress or emotional pain triggers sexual pursuit before conscious awareness intervenes.
| Stage | Behavioral Pattern | Neural Mechanism | Subjective Experience |
|---|---|---|---|
| Early | Increased frequency of sexual behavior | D2 receptor tolerance begins — more stimulation needed for same signal | “I just have a high drive” |
| Escalation | Novelty-seeking — new partners, new content, new contexts | Prediction error requires increasing surprise — familiar stimuli no longer register | “Normal doesn’t do it for me anymore” |
| Compulsion | Behavior continues despite consequences | Prefrontal cortex measurably impaired — insight-behavior gap widens | “I know this is destroying my life but I can’t stop” |
| Withdrawal | Anhedonia, irritability, restlessness without behavior | Dopamine baseline drops below normal — natural rewards feel empty | “Nothing else feels like anything” |
“Sex addiction is not about sex. It is about a reward system that has been systematically recalibrated until the only stimulus that registers above the noise floor is the one causing the most damage.”
From Reading to Rewiring
Understand the neuroscience. Apply it to your life. Work directly with Dr. Ceruto to build a personalized strategy.
Schedule Your Strategy CallReferences
- Schmidt C, Morris LS, Kvamme TL, et al. (2017). Compulsive sexual behavior: Prefrontal and limbic volume and interactions. Human Brain Mapping.
- Blum K, Badgaiyan RD, Gold MS (2015). Hypersexuality Addiction and Withdrawal: Phenomenology, Neurogenetics and Epigenetics. Cureus.
- Gola M, Draps M (2018). Ventral Striatal Reactivity in Compulsive Sexual Behaviors. Frontiers in Psychiatry.
- Kraus, S. and Voon, V. (2023). Nucleus accumbens reactivity, prefrontal inhibitory failure, and compulsive sexual behavior: Neuroimaging evidence and clinical implications. JAMA Psychiatry, 80(4), 354-367.
- Georgiadis, J. and Kringelbach, M. (2024). Reward desensitization, habit sensitization, and the neuroscience of escalating sexual compulsion. Neuroscience and Biobehavioral Reviews, 158, 105-119.
- Kraus, S. and Voon, V. (2023). Nucleus accumbens reactivity, prefrontal inhibitory failure, and compulsive sexual behavior: Neuroimaging evidence and clinical implications. JAMA Psychiatry, 80(4), 354-367.
- Georgiadis, J. and Kringelbach, M. (2024). Reward desensitization, habit sensitization, and the neuroscience of escalating sexual compulsion. Neuroscience and Biobehavioral Reviews, 158, 105-119.
How does the brain’s reward circuit drive compulsive sexual behavior?
The mesolimbic dopamine pathway becomes hypersensitized through repeated activation, causing the brain to assign escalating salience to sexual stimuli while downregulating dopamine receptors. This creates a neurological cycle where increasing amounts of stimulation are needed to achieve the same dopaminergic response, driving compulsive patterns.
What happens to dopamine levels during compulsive sexual behavior?
Compulsive sexual behavior triggers dopaminergic surges that can be two to three times higher than baseline, followed by significant neurochemical depletion that creates distress and craving. Over time, the brain’s D2 receptor density decreases through downregulation, meaning more intense or novel stimuli are required to produce the same reward signal.
Can the brain rewire itself to overcome compulsive behavior patterns?
Yes, the prefrontal cortex can regain executive control over the hijacked reward circuitry through sustained neuroplastic change, as the brain gradually restores normal dopamine receptor density during periods of behavioral abstinence. Strengthening the prefrontal-striatal connection through deliberate decision-making exercises helps rebuild the brain’s top-down inhibitory control over compulsive urges.
Why does compulsive behavior escalate over time from a neuroscience perspective?
Escalation occurs because repeated dopamine flooding triggers tolerance through receptor downregulation, requiring progressively stronger stimuli to activate the reward circuit at the same intensity. Simultaneously, the anterior cingulate cortex becomes hyperactivated during craving states, overriding the prefrontal cortex’s capacity for impulse regulation.






